Atopic Dermatitis
Relieve and Manage Chronic Inflammatory Skin with Confidence
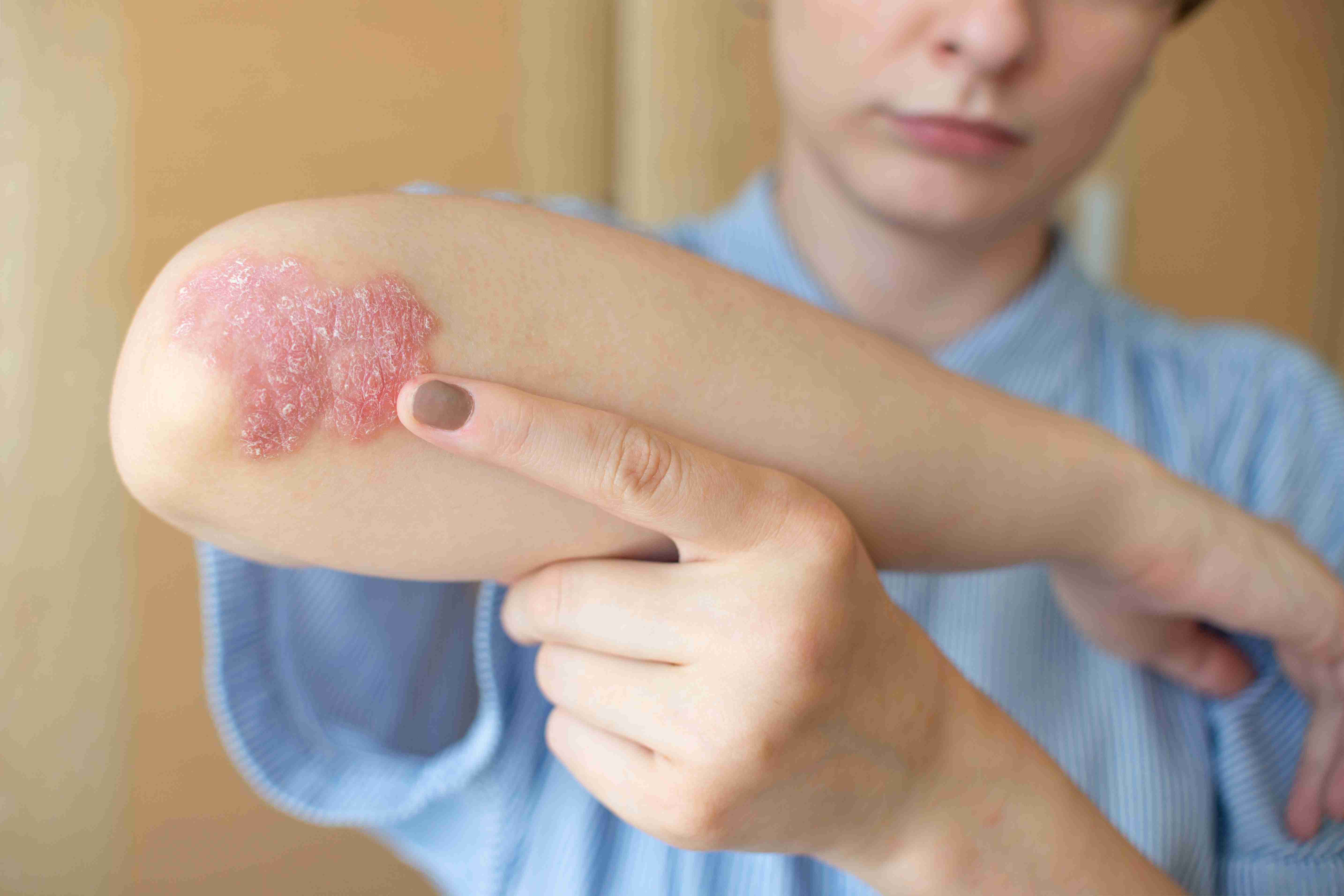
What is Atopic Dermatitis?
Atopic dermatitis is a chronic, relapsing form of eczema that causes dry, itchy, inflamed skin. It often begins in childhood but can persist or start in adulthood. This condition is linked to an overactive immune response and a weakened skin barrier, making skin vulnerable to irritation, infection, and allergens. While not contagious, it requires ongoing care.
Atopic dermatitis is driven by a combination of genetic predisposition, immune dysregulation, and environmental exposure. The condition involves an imbalance in the Th2 immune pathway, which produces excess IL-4, IL-13, and IL-31 — cytokines that fuel both inflammation and the relentless itch that characterizes atopic dermatitis.
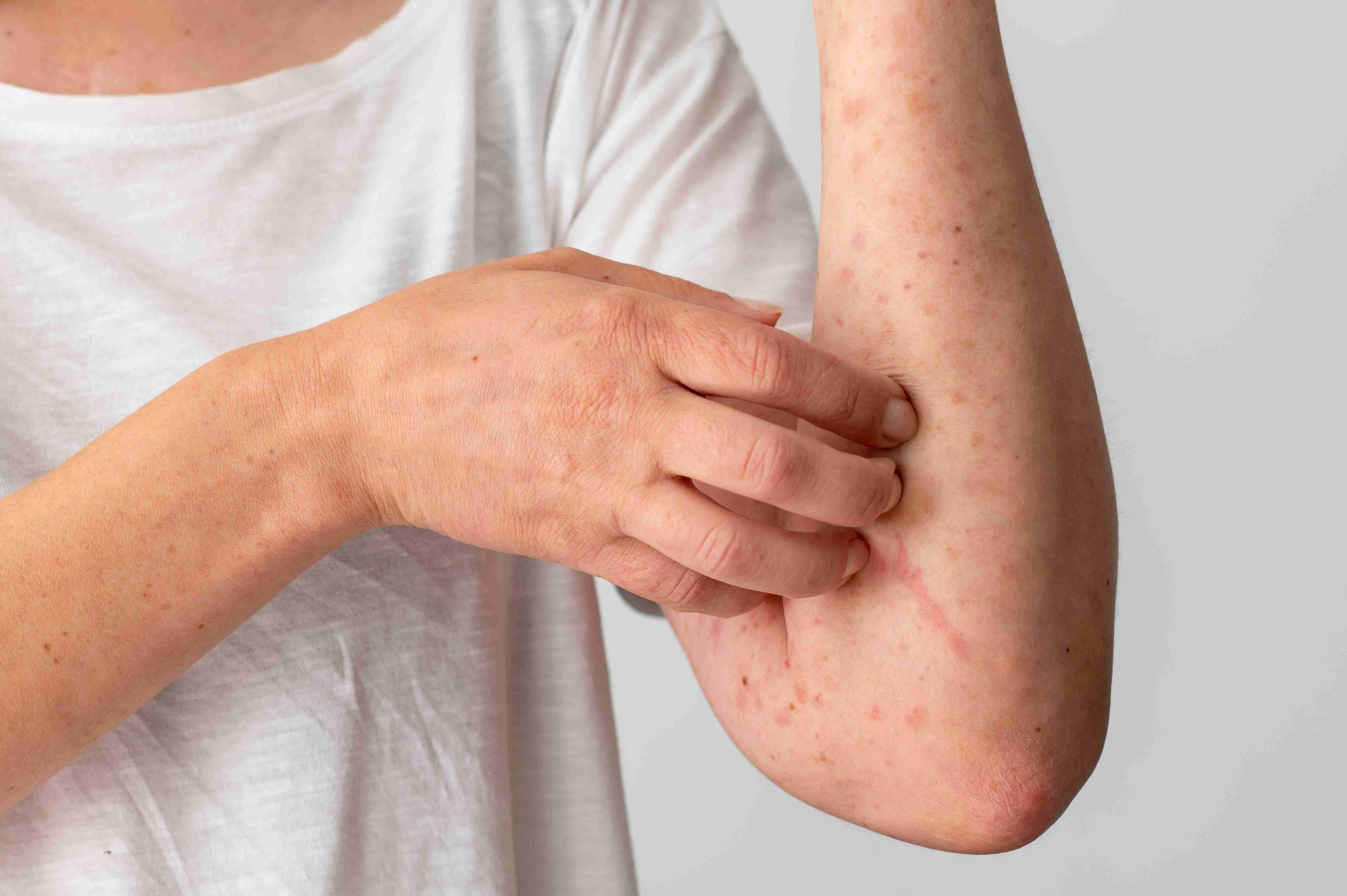
Treatment Options
Working with a dermatologist transforms atopic dermatitis management from a cycle of reactive flare treatment into a proactive strategy for sustained control. At Claire Derma, we track disease severity with validated tools at every visit, allowing us to detect early worsening before a full flare develops.
Treatment Options for Atopic Dermatitis
Diagnostic Biopsy
A biopsy confirms whether your rash is truly atopic dermatitis or something that mimics it. The distinction matters because treatment approaches vary significantly between conditions.

Hyaluronic Skin Treatments
Deep hydration therapy rebuilds the damaged skin barrier that atopic dermatitis breaks down. A stronger barrier means less moisture loss, less itching, and fewer flare-ups overall.

Skin Brightening Treatments
The repeated inflammation of atopic dermatitis leaves dark patches long after a flare clears up. Brightening treatments gently fade this discolouration and even out the skin tone.
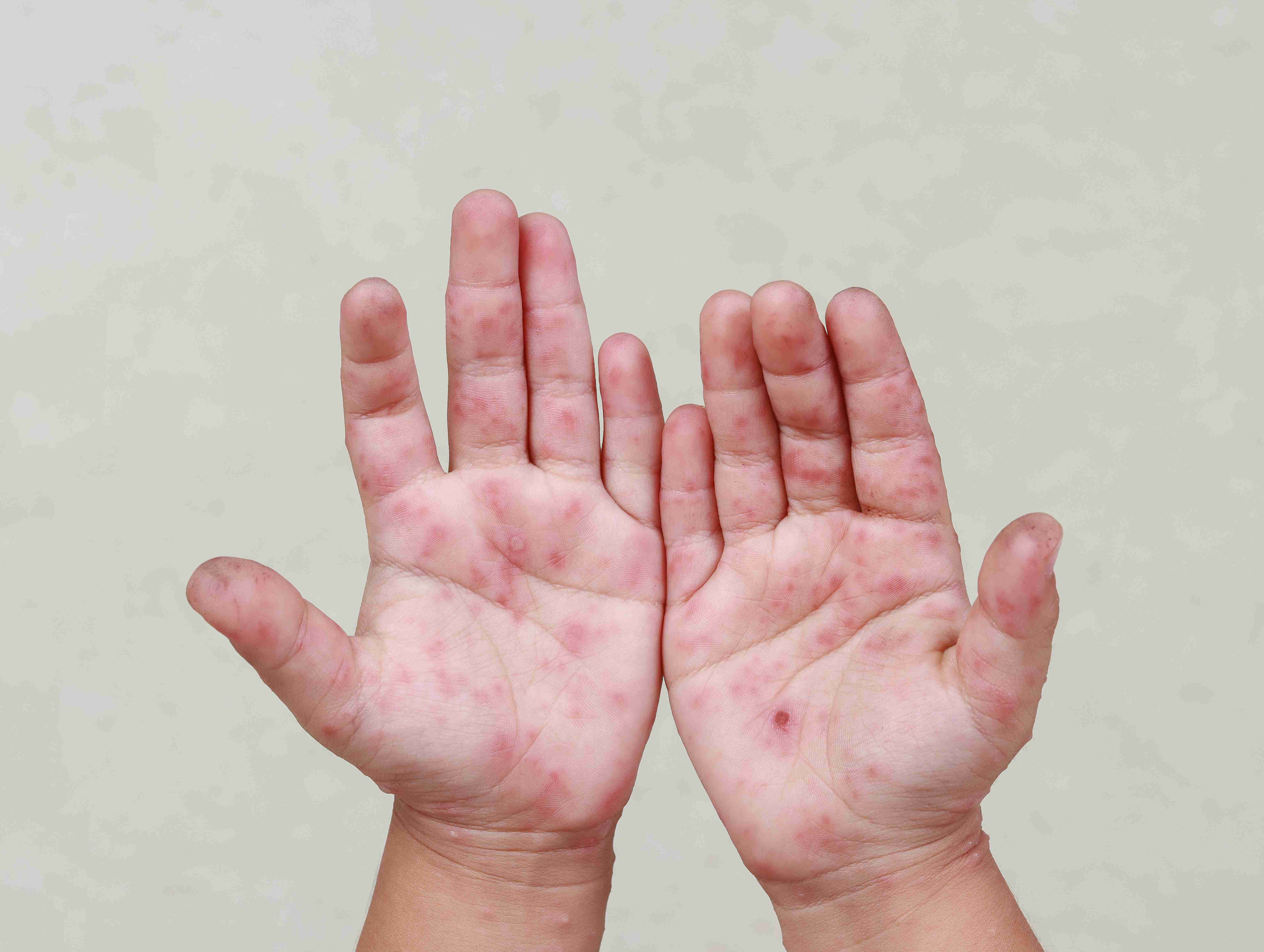
Who is at Risk?
Infants, children, and adults with a personal or family history of eczema, asthma, or hay fever are more likely to develop atopic dermatitis. It may begin in infancy and often improves with age, though it can persist or reoccur in adulthood.
Atopic dermatitis is the most common chronic inflammatory skin disease, affecting an estimated 7-10% of adults and up to 25% of children globally. It is most prevalent in industrialized nations and urban environments, a trend attributed to reduced microbial diversity in early childhood — the hygiene hypothesis. Those with a first-degree relative who has atopic dermatitis, asthma, or hay fever carry a substantially higher risk.
Treatment Flow
01
Consultation & Skin Evaluation
Assessment of skin history, allergy tendencies, and current symptoms. At your atopic dermatitis consultation, our dermatologist performs a full-body skin examination and calculates your SCORAD or EASI score to objectively measure disease severity. We document your flare frequency, known triggers, family atopic history, and any previous treatments.
02
Prescription Regimen
Anti-inflammatory creams and moisturizers prescribed for short and long-term use. We begin with a structured skin barrier repair protocol: a fragrance-free, ceramide-based emollient applied within three minutes of bathing, lukewarm showers limited to ten minutes, and removal of known irritants from your routine.
03
Lifestyle & Trigger Guidance
Identify environmental, dietary, and clothing triggers and how to avoid them. Depending on severity, your treatment at Claire Derma may include topical corticosteroids in a pulse regimen, calcineurin inhibitors for sensitive areas, phototherapy two to three times weekly, or biologic or oral systemic agents for refractory disease.
04
Monitoring & Flare Management
Regular follow-ups to adapt treatment and prevent flare-ups. Follow-up appointments are scheduled every four weeks during the active treatment phase. We repeat severity scoring, compare against your baseline photographs, and assess itch levels using a numeric rating scale. Once stable, visits move to every eight to twelve weeks for maintenance.
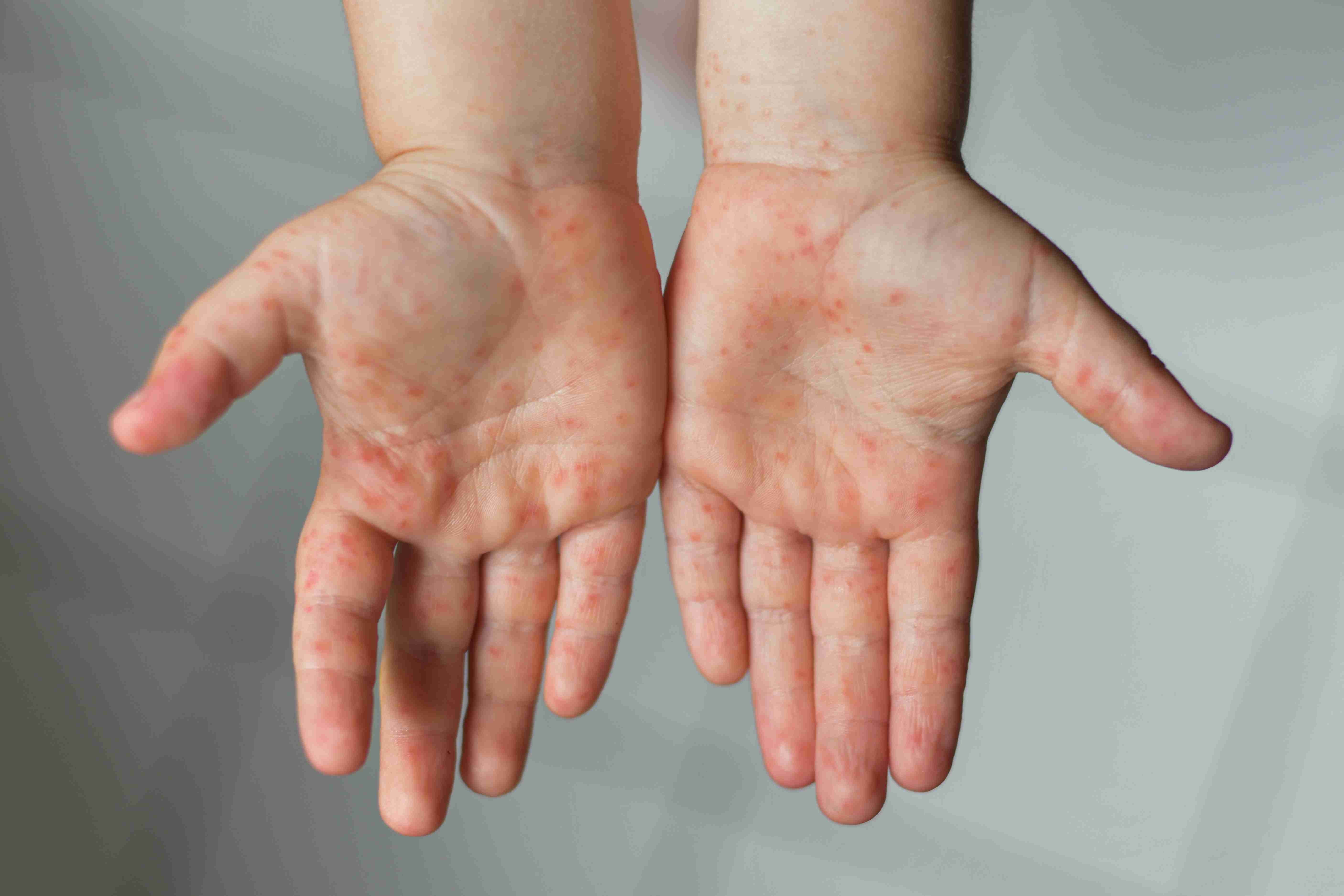
Results & Relief
Symptoms reduce within days of starting proper care.
Fewer flare-ups with long-term skin hydration and care.
Skin regains normal texture and tone over time.
Got Questions?We've Got Answers
Find answers to the most common questions about our treatments, procedures, and recovery process. If you can't find what you're looking for, our support team is always here to help.
Atopic dermatitis is a type of eczema. All atopic dermatitis is eczema, but not all eczema is atopic.
Many children outgrow it by adolescence, but some may continue to have symptoms into adulthood.
In some individuals, certain foods (e.g., dairy, eggs) may trigger or worsen symptoms. Allergy testing may help.
There’s no permanent cure, but proper care and medication can control symptoms and prevent flares.
Yes, scratching can lead to skin breaks and secondary bacterial infections. Prompt treatment helps avoid this.
Atopic dermatitis is the most common type of eczema, but eczema is a broader category that also includes contact dermatitis, dyshidrotic eczema, nummular eczema, and seborrheic dermatitis. Atopic dermatitis specifically refers to the chronic, relapsing form linked to the atopic triad of eczema, asthma, and hay fever. When people say eczema in casual conversation, they usually mean atopic dermatitis.
Biologic medications like dupilumab have limited safety data in pregnancy, so decisions must be made on a case-by-case basis with your dermatologist and obstetrician. Current guidelines generally advise caution rather than blanket prohibition. Some patients maintain their biologic through pregnancy under close monitoring, while others switch to safer alternatives like phototherapy or carefully selected topicals.
Cold outdoor air holds less moisture, and indoor heating strips humidity further, creating an environment that accelerates water loss from already barrier-compromised skin. This drop in ambient humidity is often the single biggest seasonal trigger for atopic dermatitis flares. Wool clothing and hot showers — both more common in winter — add additional irritation.
Response timelines vary by treatment type. Topical steroids can visibly reduce inflammation within three to five days. Calcineurin inhibitors and JAK inhibitor creams typically take one to two weeks to show effect. Phototherapy requires six to eight sessions before improvement becomes noticeable.
Start Your Personalized Skincare Plan
At ClairéDerma, we believe that healthy, radiant skinis the foundation of confidence and well-being. Ledby Dr. Mohna Chauhan, our clinic offers personalized dermatological care tailored to each patient's unique needs. With over a decade ofexperience and more than 3000 successfully treated patients,