Seborrheic Dermatitis
Flake-Free Skin & Scalp Care for Long-Term Relief

What is Seborrheic Dermatitis?
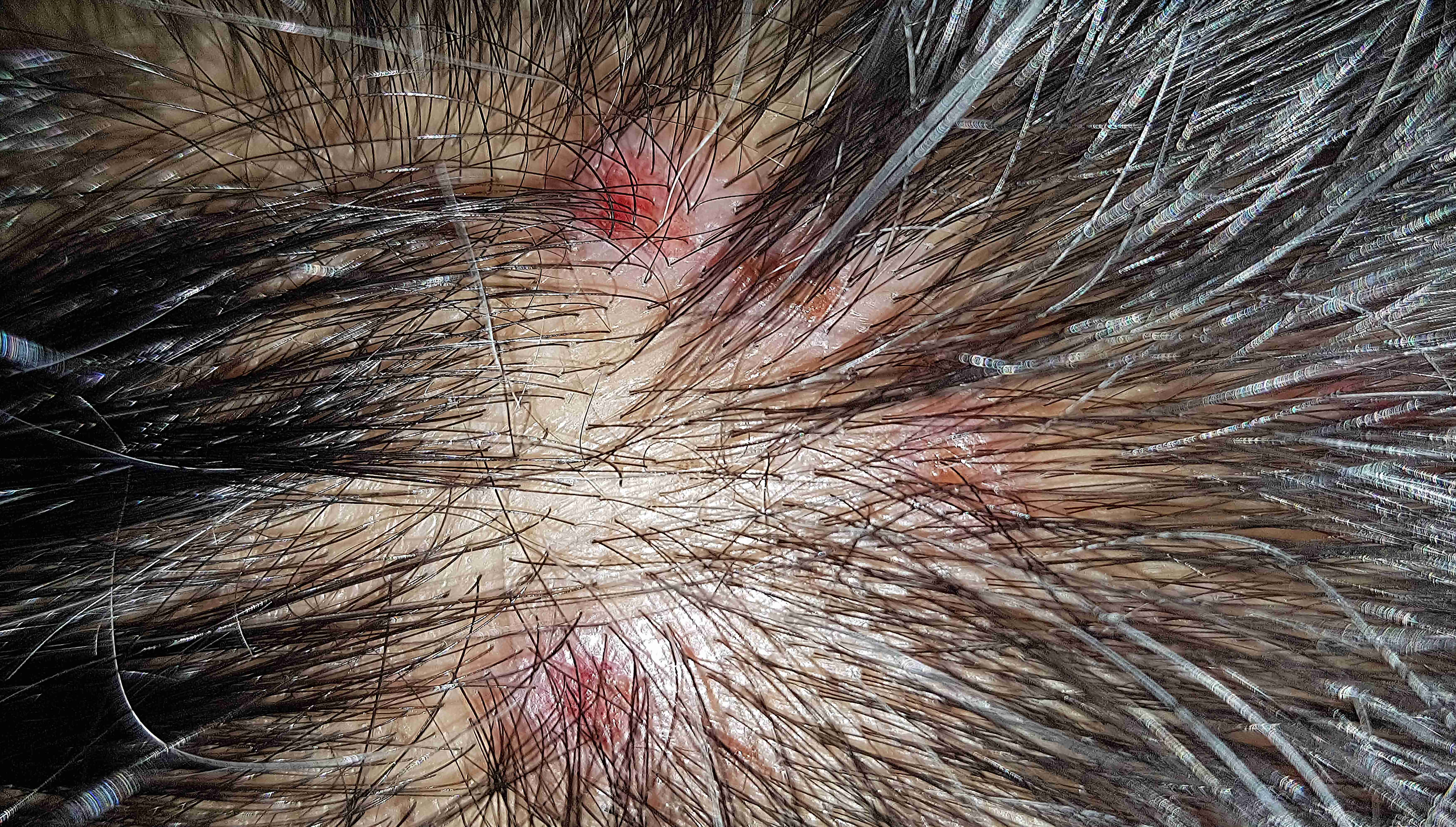
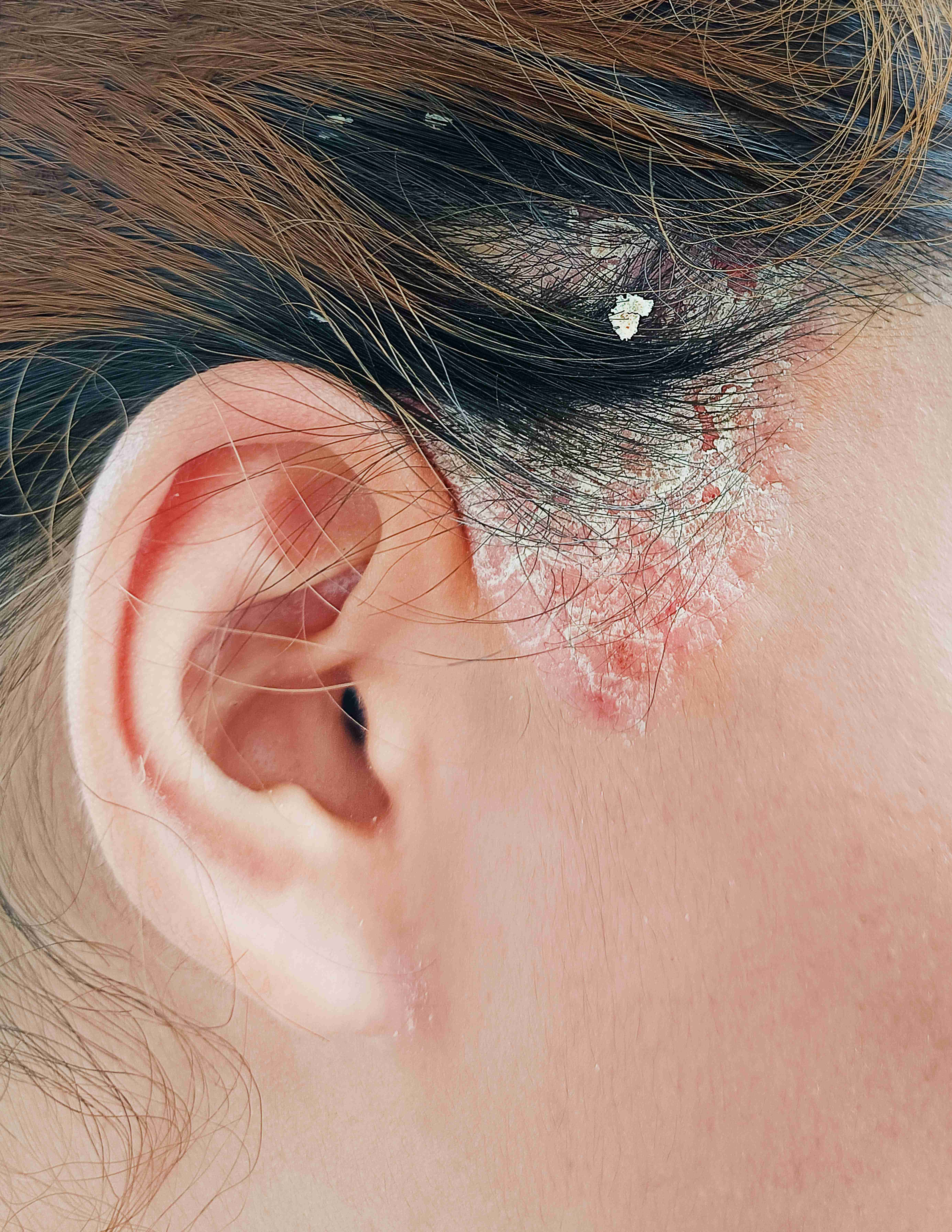
Seborrheic dermatitis is a chronic inflammatory skin condition that causes flaky, white to yellowish scales, redness, and itching. It most commonly affects oily areas such as the scalp, face (especially around the nose and eyebrows), ears, and chest. While not contagious, it can be persistent and requires regular management.
Seborrheic dermatitis arises from an abnormal immune response to Malassezia yeast, a fungus that naturally colonizes areas of skin with high sebaceous gland density. The yeast metabolizes triglycerides in sebum, producing oleic acid and other irritating byproducts that trigger inflammation in susceptible individuals.
Treatment Options
Seborrheic dermatitis is a chronic condition that waxes and wanes, and professional management ensures flares are shorter, milder, and less frequent over time. Many patients have tried multiple drugstore dandruff shampoos with inconsistent results before consulting a dermatologist.
Treatment Options for Seborrheic Dermatitis

Anti-Dandruff Treatments
Medical-grade anti-dandruff therapy targets the yeast overgrowth and flaking that define seborrheic dermatitis on the scalp. It calms the itching and reduces the greasy scales that build up.
Diagnostic Biopsy
A biopsy helps differentiate seborrheic dermatitis from psoriasis or eczema of the scalp. Getting the right diagnosis early prevents months of using the wrong treatment approach.

Skin Brightening Treatments
Seborrheic dermatitis on the face often leaves reddish-brown discolouration. Brightening treatments restore a clearer, more even tone once the active inflammation is managed.
Who Gets It?
Seborrheic dermatitis can affect people of all ages—from infants (cradle cap) to adults. It’s more common in men and individuals with oily skin, neurological disorders, or suppressed immune systems.
Seborrheic dermatitis affects approximately 3-5% of the general adult population, with higher rates among men and immunocompromised individuals. Patients with Parkinson's disease experience seborrheic dermatitis at rates between 30-80%, likely related to increased sebum production from autonomic nervous system changes. HIV-positive individuals are also disproportionately affected. Stress, fatigue, seasonal changes, and certain medications — including lithium, haloperidol, and interferon — are recognized triggers.
Treatment Flow
01
Dermatological Assessment
Visual inspection of scalp, face, or body for scaling and redness. During your seborrheic dermatitis consultation at Claire Derma, we examine all commonly affected areas — scalp, face, ears, chest, and body folds — under good lighting and magnification.
02
Prescription Treatment Plan
Antifungal shampoo, anti-inflammatory creams, and maintenance routine advised. We ask patients to discontinue any harsh or fragrant products that may be compounding irritation and switch to a gentle, sulfate-free cleanser for one to two weeks.
03
Flare-Up Management
Short course of topical steroids used during flare-ups. Your treatment plan is tailored to the affected sites. Scalp disease is addressed with medicated shampoos used two to three times weekly, while facial involvement typically calls for a topical antifungal cream combined with a calcineurin inhibitor for inflammation.
04
Maintenance & Lifestyle Advice
Long-term skincare regimen and stress management to prevent recurrence. We schedule a follow-up four to six weeks after starting treatment to assess response and adjust your antifungal rotation plan. Once controlled, maintenance visits every three to four months allow us to preemptively adapt your routine to seasonal changes.
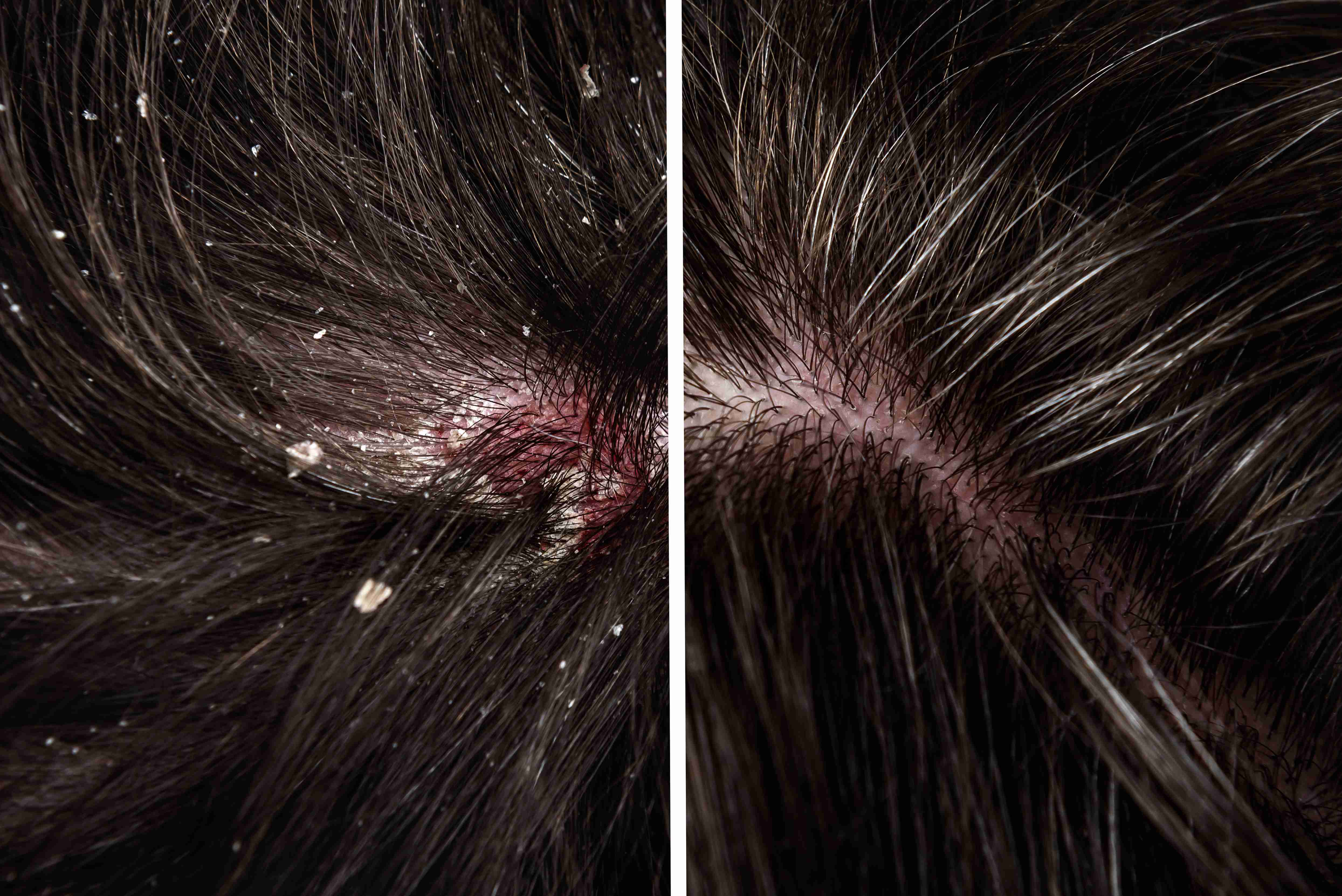
Results & Relief
Visible flake reduction within 1–2 weeks of treatment.
Redness and itching decrease with consistent care.
Flare-ups controlled with proper skin routine and triggers avoided.
Got Questions?We've Got Answers
Find answers to the most common questions about our treatments, procedures, and recovery process. If you can't find what you're looking for, our support team is always here to help.
No, it is not contagious and cannot be passed from one person to another.
Dandruff is a milder form of seborrheic dermatitis limited to the scalp.
Medicated antifungal or anti-inflammatory shampoos are more effective in managing symptoms.
Diet may not directly cause it, but overall skin health can benefit from a balanced, anti-inflammatory diet.
It’s a chronic condition, but symptoms can be effectively controlled and minimized with proper care.
Stress and poor sleep both suppress immune regulation while simultaneously increasing cortisol and sebum production — a combination that creates ideal conditions for Malassezia overgrowth and the inflammatory response it triggers. The relationship is bidirectional: flares cause self-consciousness and poor sleep, which then worsen the skin further.
Yes, but apply conditioner only to the mid-lengths and ends of your hair, keeping it away from the scalp where Malassezia thrives. Choose fragrance-free, lightweight formulas rather than heavy, oil-based conditioners that can feed yeast growth. On medicated shampoo days, let the active shampoo sit on your scalp for three to five minutes before rinsing, then follow with conditioner on the hair only.
Seborrheic dermatitis is a chronic, relapsing condition for most adult patients, meaning it can be well controlled but not permanently cured. The good news is that with the right maintenance routine, many patients go months between flares and find that each episode becomes milder and shorter than the last.
Start Your Personalized Skincare Plan
At ClairéDerma, we believe that healthy, radiant skinis the foundation of confidence and well-being. Ledby Dr. Mohna Chauhan, our clinic offers personalized dermatological care tailored to each patient's unique needs. With over a decade ofexperience and more than 3000 successfully treated patients,