Psoriasis
Soothe Chronic Inflammation and Restore Skin Confidence
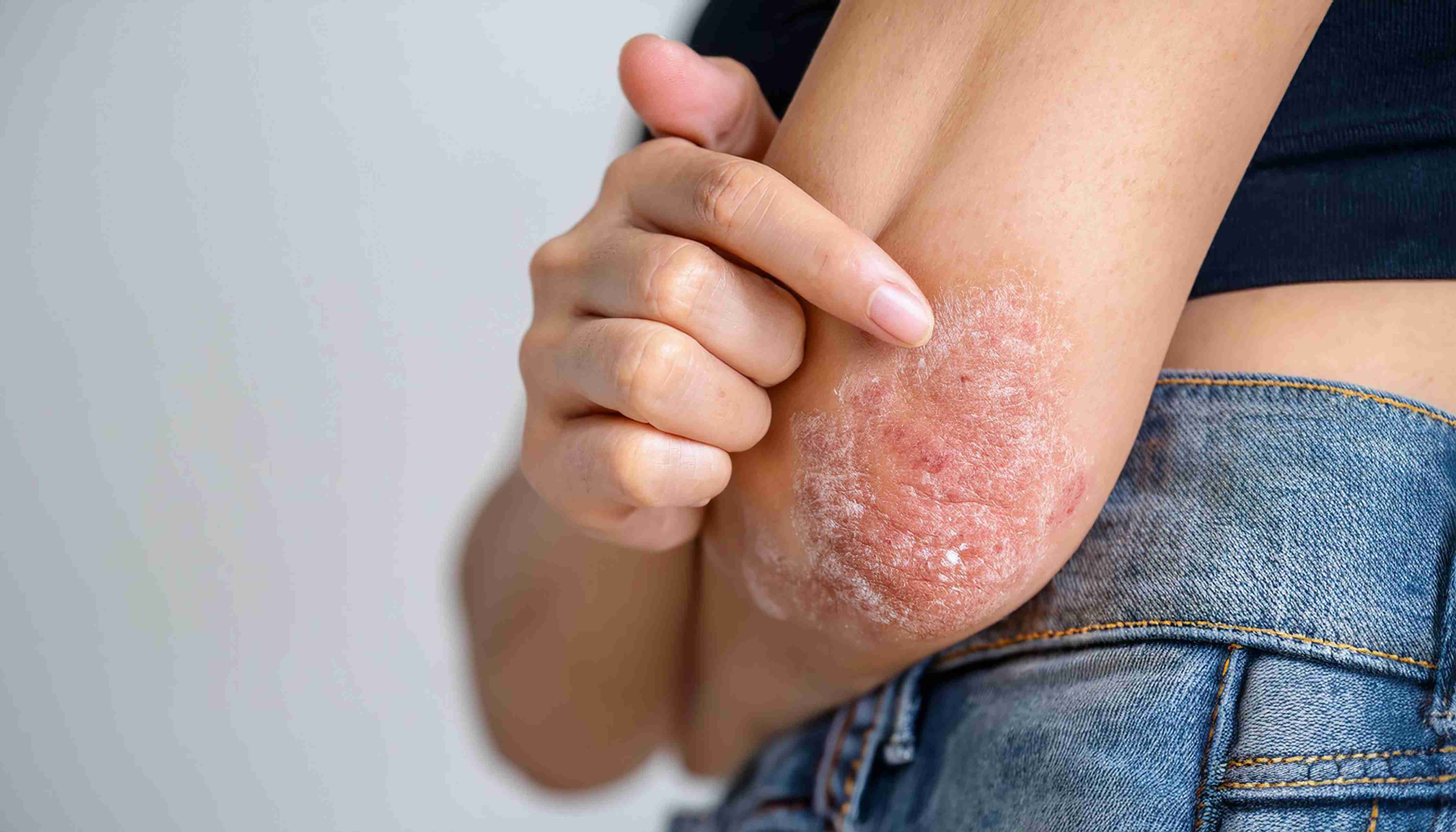
What is Psoriasis?
Psoriasis is a chronic autoimmune skin condition that causes the rapid buildup of skin cells, leading to scaling, redness, inflammation, and itchiness. The most common form is plaque psoriasis, which presents as thick, silvery-white scales over red patches. Psoriasis can affect the scalp, elbows, knees, back, nails, and even joints in some cases. It is not contagious, but it requires consistent long-term management.
Psoriasis is a systemic autoimmune condition in which T-cells mistakenly attack healthy skin cells, accelerating the cell turnover cycle from its normal 28-30 days down to just 3-4 days. This rapid proliferation creates the thick, silvery-white plaques that define the disease.
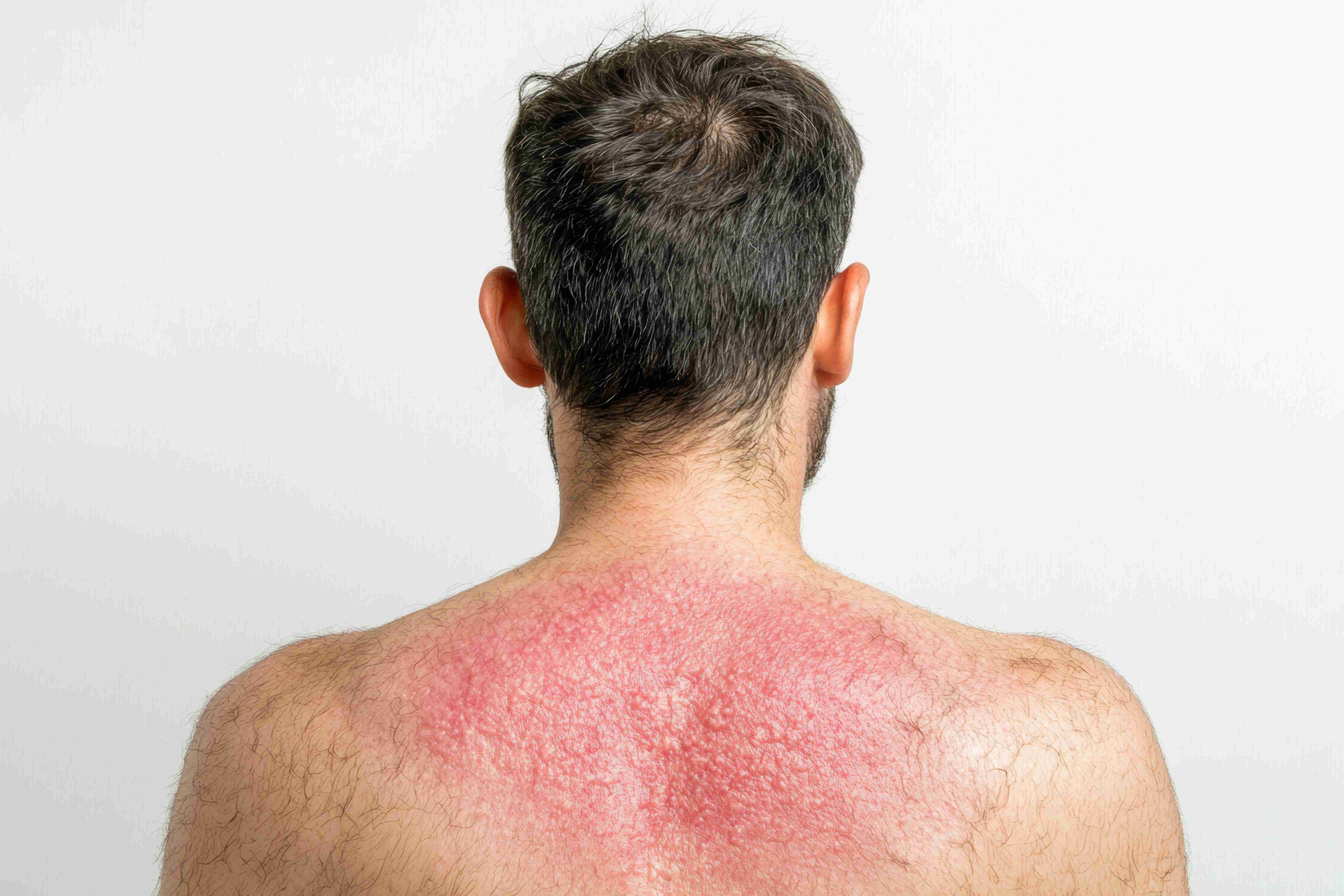
Treatment Options
Dermatologist-led psoriasis management changes the disease trajectory in ways that self-treatment cannot. At Claire Derma, we screen for psoriatic arthritis at every visit because early detection prevents irreversible joint damage. We monitor metabolic markers including lipid profiles and fasting glucose, since psoriasis patients carry elevated cardiovascular risk.
Treatment Options for Psoriasis

Laser Treatments
Targeted laser therapy slows the rapid skin cell growth that causes psoriasis plaques. It focuses only on affected areas, sparing healthy skin and reducing plaque thickness and redness.
Diagnostic Biopsy
A biopsy confirms psoriasis and helps distinguish it from similar-looking conditions. This is especially useful when the presentation is unusual or does not respond to standard treatments.

Skin Brightening Treatments
After psoriasis plaques clear, they often leave behind stubborn dark marks. Brightening treatments help fade these post-inflammatory patches and bring back a more uniform complexion.

Who is Affected?
Psoriasis can affect individuals of any age, but it is most commonly diagnosed between the ages of 15 and 35. It affects men and women equally and is more likely in people with a family history of autoimmune or skin disorders.
Psoriasis affects approximately 2-3% of the global population, with onset typically occurring in two peak age windows: between 15 and 25 years old, and again between 50 and 60. A strong genetic component exists — having one parent with psoriasis gives a child a roughly 10% chance of developing the condition, rising to 50% if both parents are affected.
Treatment Journey
01
Dermatological Assessment
Diagnosis based on clinical features and, if needed, a skin biopsy. At your psoriasis consultation, our dermatologist performs a full-body skin examination, calculates your body surface area involvement and PASI score, and checks for nail and joint involvement.
02
Customized Treatment Planning
Treatment is tailored to the severity, location, and patient’s health profile. For patients starting biologic or systemic therapy, preparation includes screening blood work — complete blood count, hepatic and renal function, hepatitis B and C serology, and tuberculosis testing.
03
Active Treatment Phase
Use of topicals, systemics, biologics, or phototherapy to control symptoms. Treatment is matched to disease severity and patient preference. Options at Claire Derma include topical steroids with vitamin D analogues, narrowband UVB phototherapy two to three times weekly, oral agents like methotrexate or apremilast, and biologic injections targeting TNF-alpha, IL-17, or IL-23.
04
Long-Term Management
Maintenance therapy and lifestyle modifications to reduce flare-ups. Follow-up visits occur every eight to twelve weeks during active treatment. We reassess your PASI score, screen for psoriatic arthritis symptoms, review lab work for patients on systemic agents, and discuss any side effects or adherence challenges.
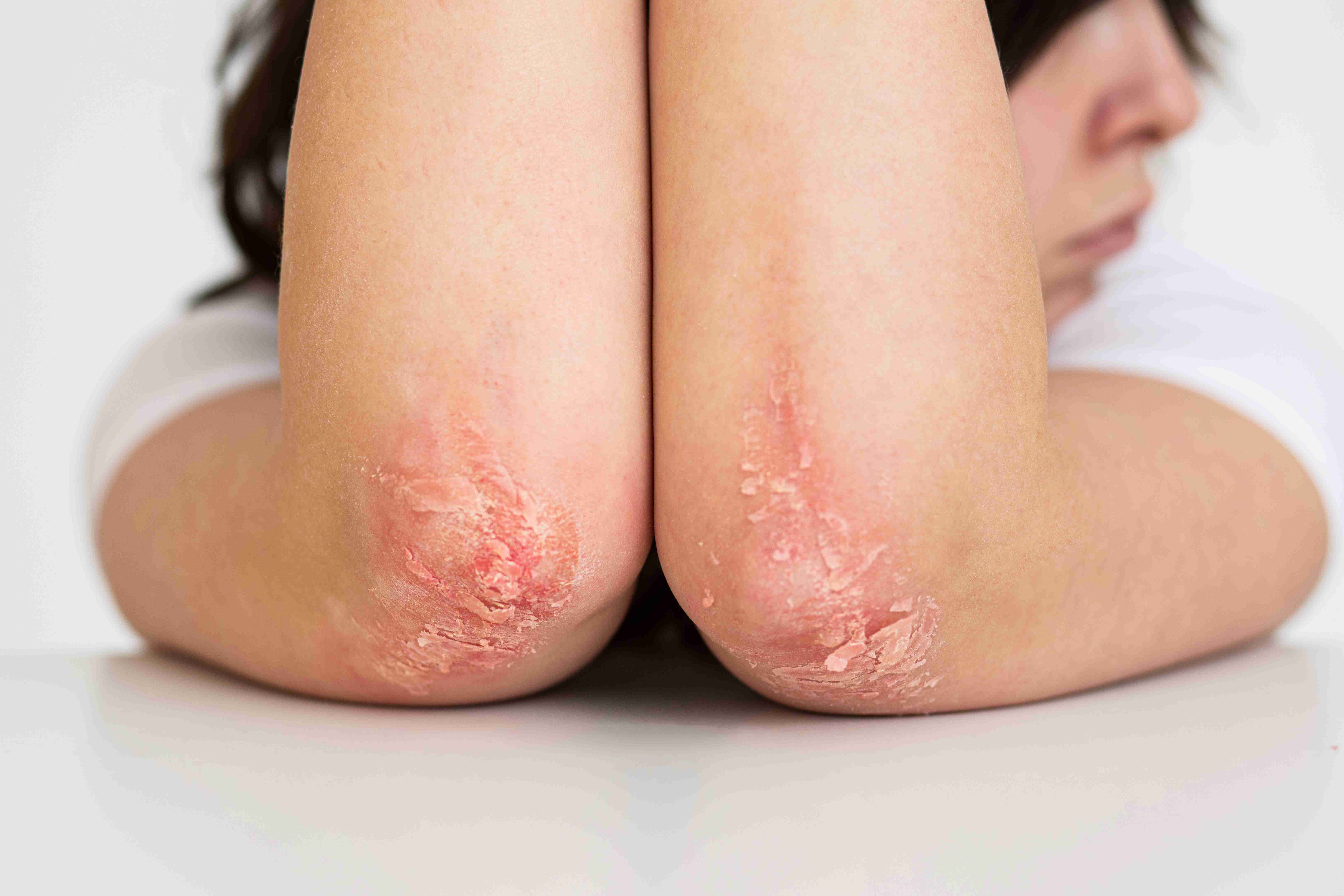
Expected Results
Visible reduction in scaling and redness with consistent treatment.
Improved skin appearance, comfort, and confidence.
Fewer flare-ups with long-term adherence and dermatologist guidance.
Got Questions?We've Got Answers
Find answers to the most common questions about our treatments, procedures, and recovery process. If you can't find what you're looking for, our support team is always here to help.
No, psoriasis is not contagious and cannot be passed through touch or contact.
There is no permanent cure, but long-term remission and symptom control are possible with appropriate treatment.
Yes, stress is a common trigger and managing stress is an important part of psoriasis care.
While diet isn’t a direct cause, anti-inflammatory foods may help reduce flares in some individuals.
Yes, about 30% of psoriasis patients may develop psoriatic arthritis, which causes joint stiffness and swelling.
Some patients experience sustained remission lasting months or years, particularly after successful biologic therapy, but psoriasis is a chronic condition with no permanent cure. Certain biologics demonstrate durable responses — some patients maintain clear skin even after extending the interval between injections. At Claire Derma, we aim for the longest possible remission with the least treatment burden.
Biologic therapies have been used for psoriasis since the early 2000s, and we now have over twenty years of safety data for the earliest agents and growing real-world experience with newer ones. Long-term registry studies show that the overall risk profile remains stable with continued use.
Psoriasis is increasingly recognized as a systemic inflammatory condition rather than a purely skin disease. The chronic inflammation that drives skin plaques also affects blood vessels and metabolic processes. Patients with moderate-to-severe psoriasis have higher rates of heart disease, type 2 diabetes, obesity, fatty liver disease, and depression. Psoriatic arthritis develops in roughly 30% of cases.
Research supports a meaningful connection between body weight and psoriasis severity. Adipose tissue produces inflammatory cytokines that overlap with those driving psoriasis, so excess weight can worsen the condition and reduce the effectiveness of treatment.
Start Your Personalized Skincare Plan
At ClairéDerma, we believe that healthy, radiant skinis the foundation of confidence and well-being. Ledby Dr. Mohna Chauhan, our clinic offers personalized dermatological care tailored to each patient's unique needs. With over a decade ofexperience and more than 3000 successfully treated patients,