Vitiligo
Restore Pigment, Rebuild Confidence

What is Vitiligo?
Vitiligo is a long-term skin condition in which the body loses melanocytes—the cells responsible for producing melanin, the pigment that gives skin its color. This results in white patches of skin that may appear anywhere on the body, including the face, hands, feet, arms, and genitals. While vitiligo is not harmful or contagious, it can impact a person’s emotional well-being and confidence.
Vitiligo results from the immune system attacking and destroying melanocytes, the cells responsible for producing melanin. The exact trigger remains under investigation, but current evidence points to a combination of genetic susceptibility, oxidative stress within melanocytes, and autoimmune dysregulation. Over 70 gene loci have been linked to vitiligo risk, many of which overlap with genes involved in other autoimmune conditions like thyroid disease and type 1 diabetes.

Treatment Options for Vitiligo
Structured vitiligo treatment at Claire Derma gives patients measurable progress they can track over time. Phototherapy combined with topical agents achieves meaningful repigmentation in 60 to 70 percent of patients with facial and neck vitiligo, and 40 to 50 percent for body sites.
Treatment Options for Vitiligo

Laser Treatments
Targeted laser therapy stimulates the remaining melanocytes in depigmented patches, encouraging them to produce pigment again. Consistent sessions can bring colour back to affected areas.

Skin Brightening Treatments
Brightening treatments help even out the contrast between vitiligo patches and surrounding skin. The goal is to create a more uniform appearance while supporting repigmentation.
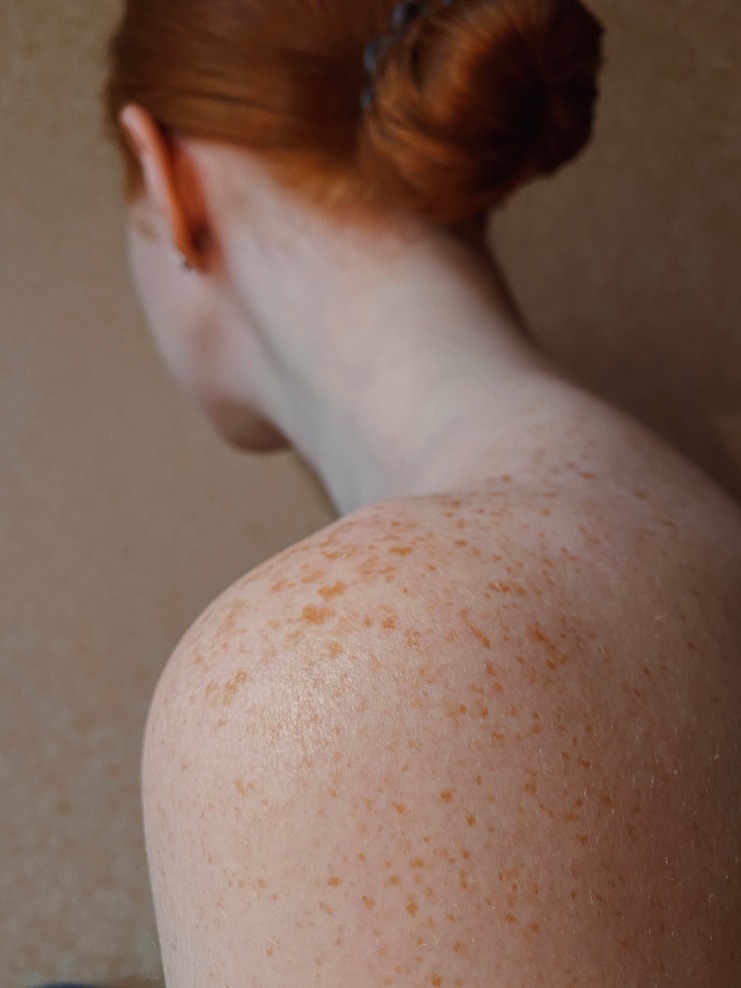
Diagnostic Biopsy
A skin biopsy helps confirm the vitiligo diagnosis and rule out other conditions that look similar. Getting the right diagnosis early means the treatment plan can be more precise from the start.
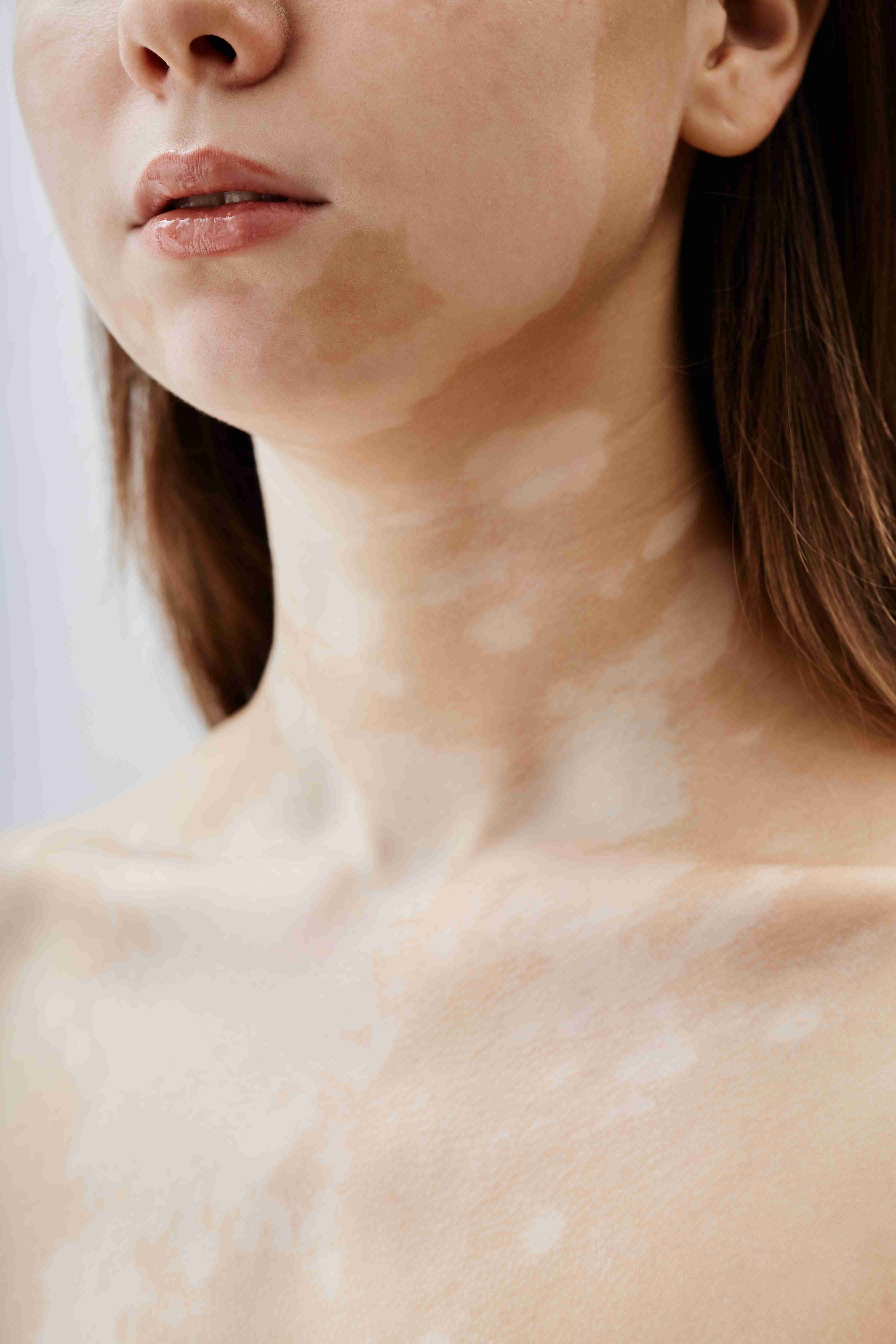
Who is Affected?
Vitiligo can affect people of all skin types and ages, though it is more noticeable in individuals with darker skin. It often begins before the age of 30 and may be associated with other autoimmune disorders such as thyroid disease or alopecia areata.
A personal or family history of autoimmune disease — thyroid conditions, alopecia areata, rheumatoid arthritis, or type 1 diabetes — is the strongest predictor of vitiligo risk. Severe sunburns, chemical exposure to phenolic compounds (found in some hair dyes and industrial cleaners), and significant emotional stress have all been reported as triggers for new patches in genetically susceptible individuals.
Treatment Journey
01
Diagnosis
Visual examination, Wood’s lamp test, and medical history assessment are done to confirm vitiligo. Our dermatologist performs a full-body skin examination under Wood's lamp to map all depigmented and subclinical areas. Your medical and family history is reviewed, activity of the disease is assessed, and blood tests for thyroid function and vitamin B12 are ordered.
02
Initial Treatment
Topical medications or phototherapy are initiated based on patch size and location. Based on activity status, topical tacrolimus or corticosteroids are prescribed to stabilise active patches before phototherapy begins. Patients receive guidance on strict sun protection — SPF 50+ sunscreen on depigmented areas daily — to prevent sunburn and reduce the contrast between affected and unaffected skin.
03
Advanced Options
In resistant or stable vitiligo, surgical repigmentation may be considered. Narrowband UVB sessions are scheduled two to three times per week, each lasting one to five minutes depending on skin type and dose protocol. Treatments are combined with continued topical immunomodulators. Progress photographs are taken every eight weeks.
04
Ongoing Support
Regular review, skincare advice, and psychological support are provided throughout treatment. Repigmentation is assessed at eight-week intervals using standardised photography and Wood's lamp. Treatment intensity is adjusted based on response — responders continue until maximum improvement plateaus, while non-responders are offered alternative approaches including melanocyte transfer. Thyroid and B12 levels are rechecked annually.

Results & Expectations
Early treatment leads to faster and more effective repigmentation.
Visible improvement within 2–3 months of consistent therapy.
Continued maintenance and stress reduction help prevent further spread.
Got Questions?We've Got Answers
Find answers to the most common questions about our treatments, procedures, and recovery process. If you can't find what you're looking for, our support team is always here to help.
No, vitiligo is not contagious and cannot spread through touch or contact.
There is no guaranteed cure, but treatment can effectively restore pigmentation and control spread.
Yes, emotional stress is a known trigger and may worsen or spread vitiligo in some individuals.
Vitiligo is a relapsing condition. Maintenance therapy helps sustain results and prevent recurrence.
Yes, in some cases vitiligo may cause white hair (leukotrichia) or slight pigment changes in the eyes.
Facial and neck vitiligo typically shows the earliest response — small dots of colour around hair follicles may appear within eight to twelve weeks of consistent narrowband UVB sessions. Body sites like the hands, feet, and bony areas take longer, sometimes six months or more, because they have fewer hair follicles to serve as melanocyte reservoirs.
Yes. Vitiligo shares genetic pathways with several autoimmune disorders. Up to 20 percent of vitiligo patients develop thyroid disease, and associations with alopecia areata, pernicious anaemia, and type 1 diabetes are well documented. At Claire Derma, we routinely screen for thyroid antibodies, vitamin B12 deficiency, and blood glucose abnormalities at diagnosis and during annual follow-ups.
Psychological stress does not cause vitiligo directly, but it can act as a trigger in people who carry the genetic predisposition. Stress hormones like cortisol and catecholamines influence immune regulation and may tip the balance toward melanocyte destruction in susceptible individuals. Many patients at Claire Derma report that new patches appeared during particularly stressful periods.
In most cases, repigmented skin achieves a close match to the surrounding tone, especially on the face and neck where melanocyte reservoirs in hair follicles are dense. Some patients notice a slightly lighter or darker shade initially, but this usually evens out over the following months as melanin production stabilises.
Start Your Personalized Skincare Plan
At ClairéDerma, we believe that healthy, radiant skinis the foundation of confidence and well-being. Ledby Dr. Mohna Chauhan, our clinic offers personalized dermatological care tailored to each patient's unique needs. With over a decade ofexperience and more than 3000 successfully treated patients,