Fungal Infection
Effective Relief from Itching, Redness, and Fungal Overgrowth

What is a Fungal Infection?
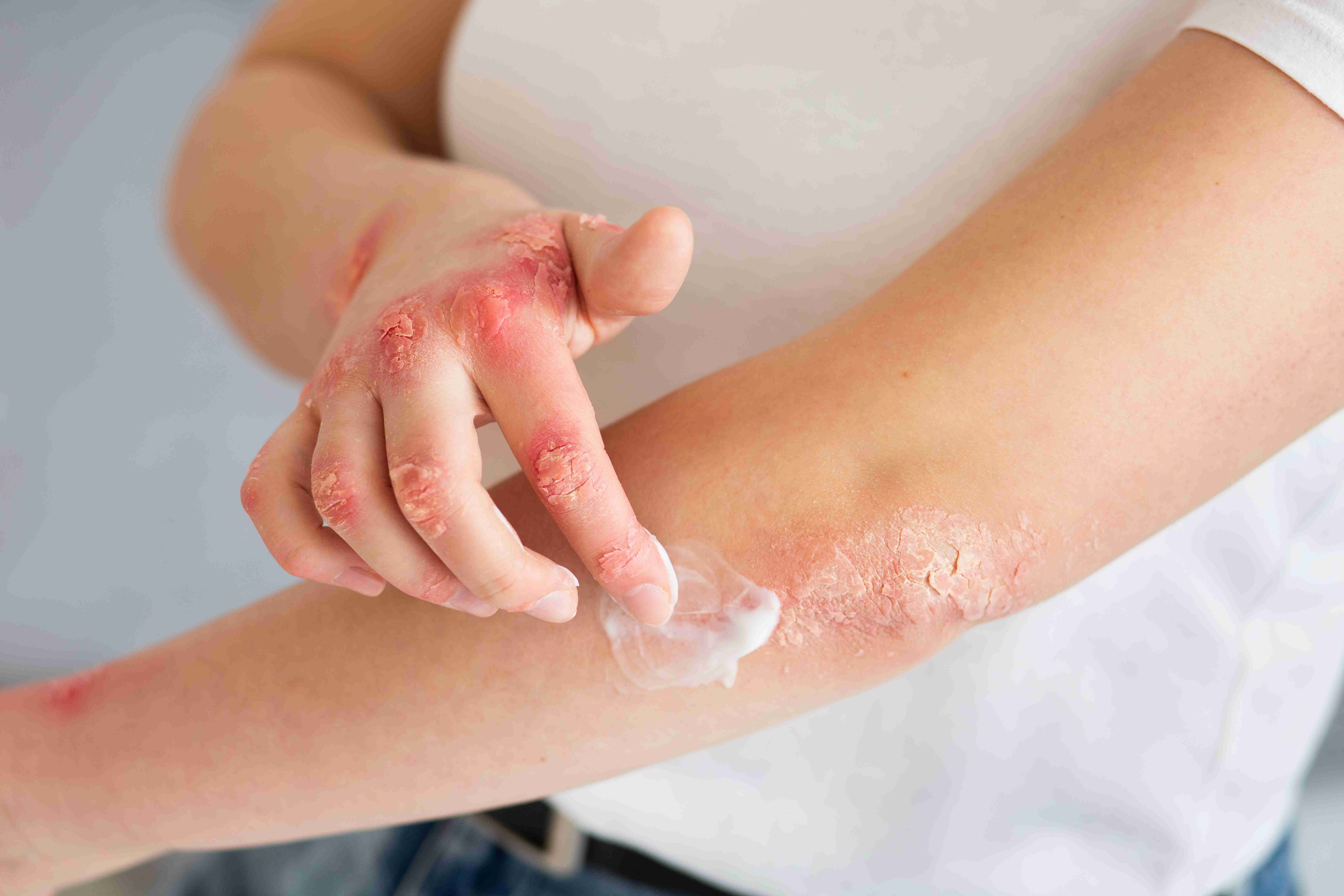
Fungal infections are caused by overgrowth of fungi on the skin, nails, or scalp. These infections are common in warm, humid climates and often affect the feet, groin, underarms, or folds of skin. Symptoms include red, itchy, scaly, and sometimes oozing patches. Though treatable, fungal infections can spread if left unchecked.
Fungal skin infections are caused by dermatophytes, yeasts, and moulds that thrive in warm, moist environments. Dermatophytes — the group responsible for ringworm, athlete's foot, and jock itch — feed on keratin in the skin, nails, and hair. Candida species prefer skin folds where sweat accumulates, while Malassezia yeast overgrowth leads to pityriasis versicolor, producing light or dark patches across the trunk.
Treatment Options
Targeted antifungal treatment from Claire Derma resolves symptoms faster and more reliably than self-medication with over-the-counter creams — which may contain the wrong active ingredient for the causative species. Proper diagnosis also prevents the common mistake of applying topical steroids to fungal infections, a practice called tinea incognito. Steroids mask the rash while letting the fungus spread unchecked.
Treatment Options for Fungal Infection
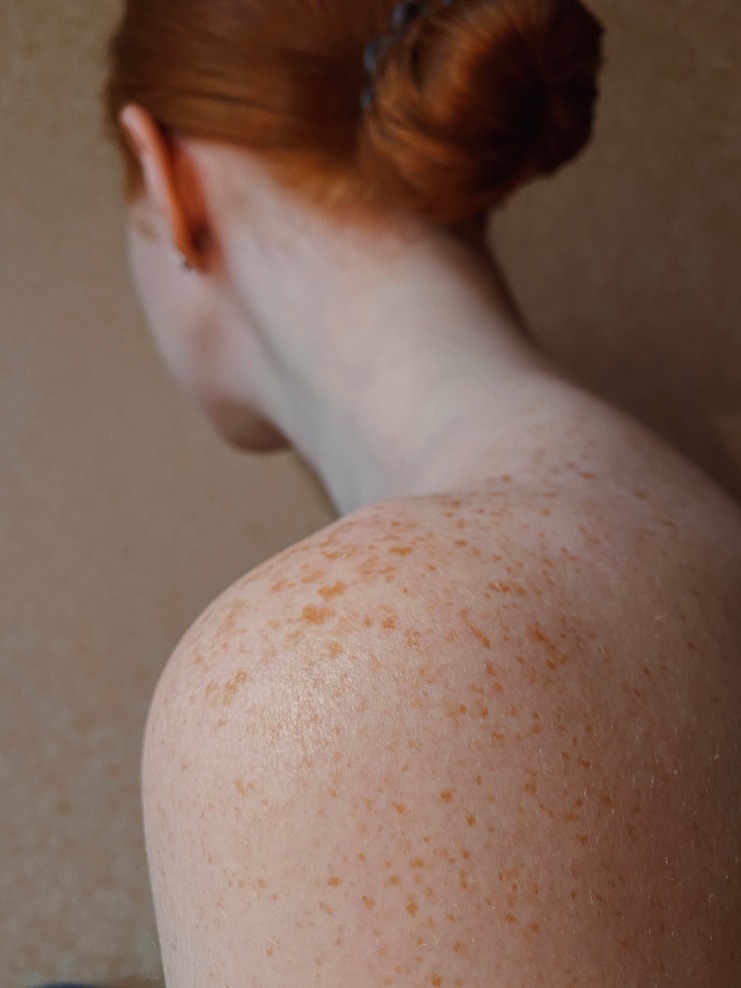
Diagnostic Biopsy
A skin scraping or biopsy identifies the exact fungus causing the infection. This matters because different fungal species respond to different antifungal medications, and guessing wastes time.

Body Polishing
Once the infection is cleared, a gentle polishing treatment removes the residual rough, discoloured skin. It leaves the affected area smoother and helps prevent reinfection by removing dead skin buildup.

Skin Brightening Treatments
Fungal infections frequently leave behind dark patches after they heal. Brightening treatments fade this post-inflammatory hyperpigmentation and restore the skin's natural colour.
Who is at Risk?
People who sweat excessively, wear tight or synthetic clothing, live in hot and humid environments, or share personal items are at higher risk. Immunocompromised individuals are also more prone to fungal infections.
Diabetes, obesity, immunosuppression, and prolonged antibiotic use all raise the risk of fungal skin infections. Sweating heavily, wearing occlusive footwear or synthetic fabrics, and working in humid environments create ideal conditions for fungal colonisation. Athletes who share locker rooms, wrestlers with direct skin-to-skin contact, and people who frequent public pools face increased exposure. A weakened skin barrier — from eczema, frequent hand washing, or macerated skin in folds — lowers the threshold for infection.
Treatment Process
01
Consultation & Diagnosis
Physical examination and possible skin scraping for lab analysis. Our dermatologist inspects the affected skin, nails, or scalp and takes a detailed history covering duration, previous treatments, and possible exposure sources. A KOH scraping or Wood's lamp exam is performed in the same visit.
02
Medication Prescription
Topical or oral antifungals prescribed depending on severity and area affected. For topical treatment, we demonstrate proper application: cleaning the area, drying thoroughly, and applying cream one centimetre beyond the visible rash border. For systemic therapy, baseline blood tests including liver enzymes are ordered.
03
Follow-up & Monitoring
Check for complete recovery and guidance on hygiene practices to prevent recurrence. Topical antifungals are applied twice daily for the prescribed duration, typically two to four weeks for skin infections. Oral therapy begins once blood results confirm safe liver function. For nail infections, amorolfine nail lacquer may be added as a topical adjunct.

Expected Results & Recovery
Got Questions?We've Got Answers
Find answers to the most common questions about our treatments, procedures, and recovery process. If you can't find what you're looking for, our support team is always here to help.
Yes, it can spread through direct contact or sharing towels, clothes, or shoes.
Home remedies may provide temporary relief but do not eliminate the infection. Medical treatment is recommended.
Most fungal infections clear up within 2–4 weeks with proper treatment.
It may, especially in hot climates or if hygiene isn’t maintained. Preventive care is key.
Yes, fungal infections can affect the scalp (tinea capitis) and nails (onychomycosis) and require specialized treatment.
Recurrence usually happens when the original course of treatment was too short, the wrong antifungal was used, or environmental factors were not addressed. Fungal spores can survive on shoes, towels, and shower floors for months, causing reinfection even after the skin appears clear. At Claire Derma, we extend treatment for at least one week beyond visual clearance and recommend disinfecting personal items.
Yes. Dermatophytes can spread from the feet to the groin via contaminated towels or hands — a pattern called tinea pedis to tinea cruris transmission. Scratching an infected area and then touching another body part transfers spores directly. Nail fungus can seed surrounding skin, and scalp fungus can spread through shared combs.
Oral terbinafine and itraconazole are well tolerated by most patients, but they are metabolised by the liver, so baseline liver function tests are standard practice at Claire Derma before prescribing them. A mid-treatment blood check confirms that enzyme levels remain normal. Serious liver reactions are rare — occurring in fewer than 1 in 50,000 patients for terbinafine.
Toenail fungus is slow to resolve because nails grow at roughly three to four millimetres per month. Oral terbinafine is taken for 12 weeks, but the nail continues to clear over six to nine months as the healthy nail replaces the damaged portion. At Claire Derma, we set this expectation upfront so patients are not discouraged by gradual progress.
Start Your Personalized Skincare Plan
At ClairéDerma, we believe that healthy, radiant skinis the foundation of confidence and well-being. Ledby Dr. Mohna Chauhan, our clinic offers personalized dermatological care tailored to each patient's unique needs. With over a decade ofexperience and more than 3000 successfully treated patients,