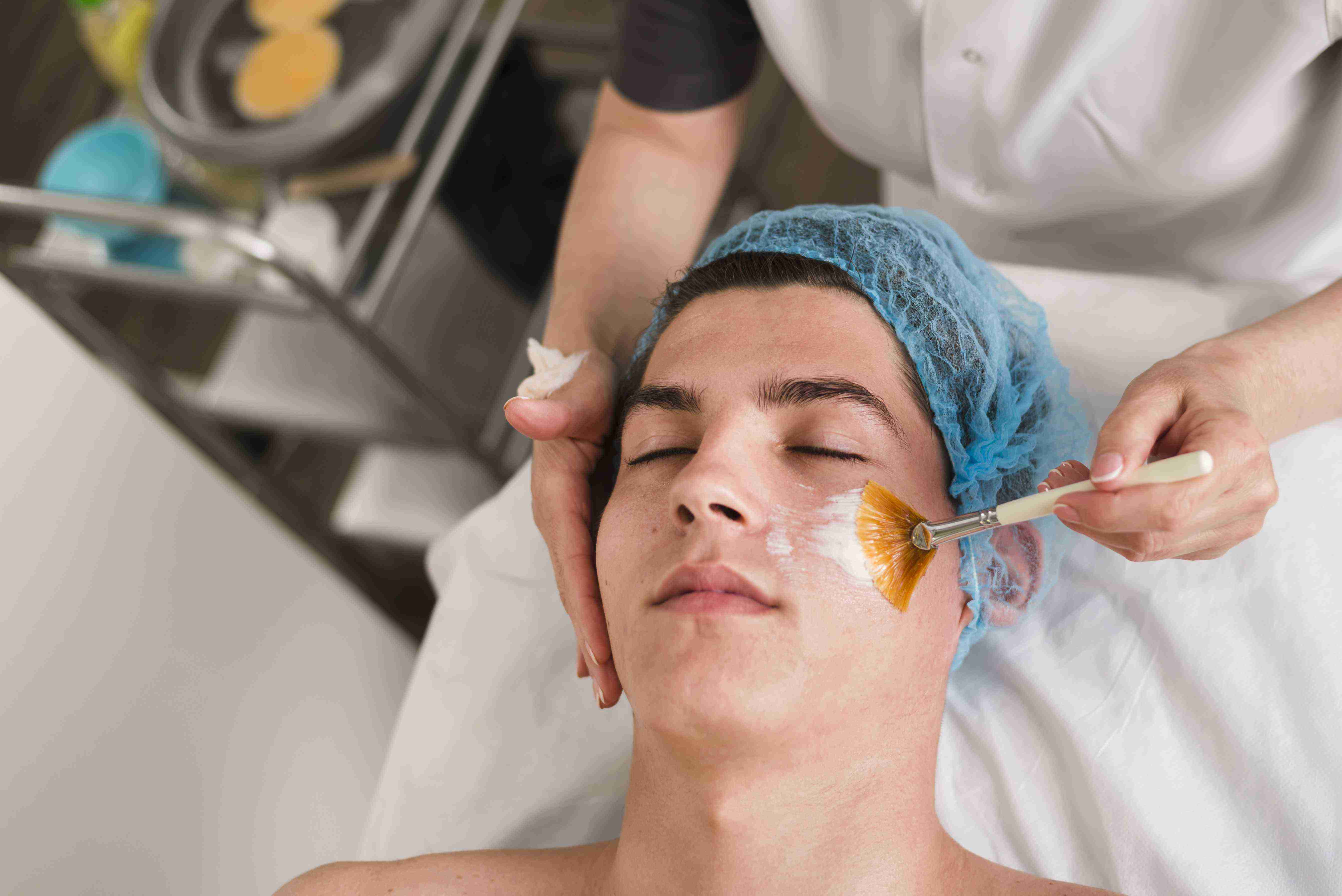
Introduction to Hair Transplant Consultation for Androgenetic Alopecia
Androgenetic Alopecia, commonly referred to as male or female pattern baldness, is a progressive condition resulting in hair thinning and eventual hair loss due to genetic and hormonal factors. A hair transplant consultation helps assess the degree of hair loss and determines the best treatment strategy to restore hair density.
Androgenetic alopecia is the most common indication for hair transplant surgery, and the consultation at Claire Derma determines whether transplantation is appropriate for your specific stage and pattern of loss. Our trichologists evaluate the stability of your donor area — the permanent horseshoe zone in the occipital and parietal scalp that resists DHT-driven miniaturisation — to estimate the total number of available grafts.
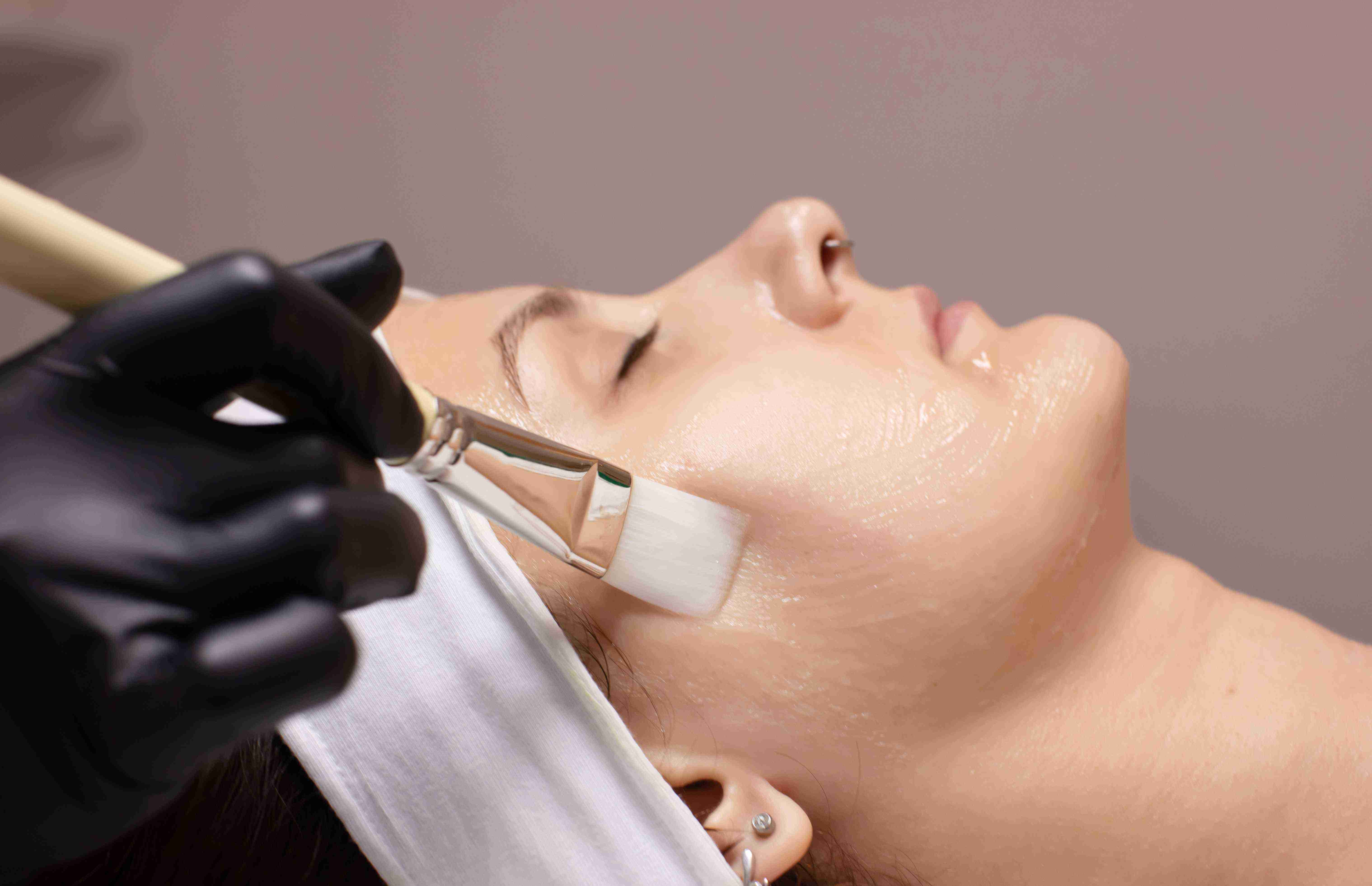
How Hair Transplant Consultation Works
These peels work by deeply penetrating the skin to:
The consultation at Claire Derma begins with a thorough scalp assessment using dermoscopy and macrophotography to classify your hair loss on the Norwood-Hamilton scale for men or the Ludwig scale for women.
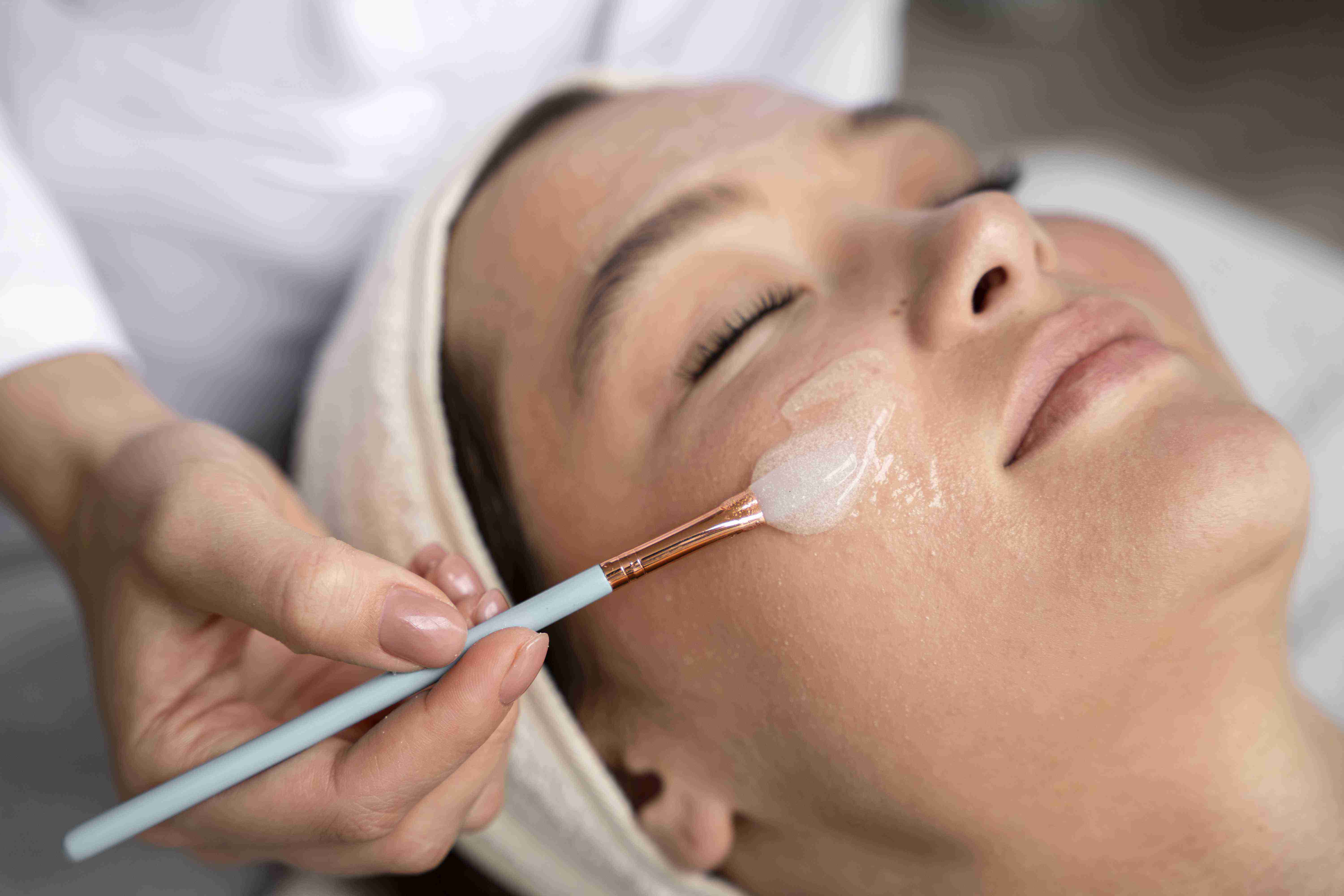
Treating Androgenetic Alopecia with Hair Transplant
During the consultation, our team at Claire Derma explains the two primary transplant techniques — Follicular Unit Extraction and Follicular Unit Transplantation — so you can make an informed decision about your procedure. FUE involves extracting individual follicular units using 0.8 to 1.0 mm circular punches, leaving tiny dot scars scattered across the donor area.
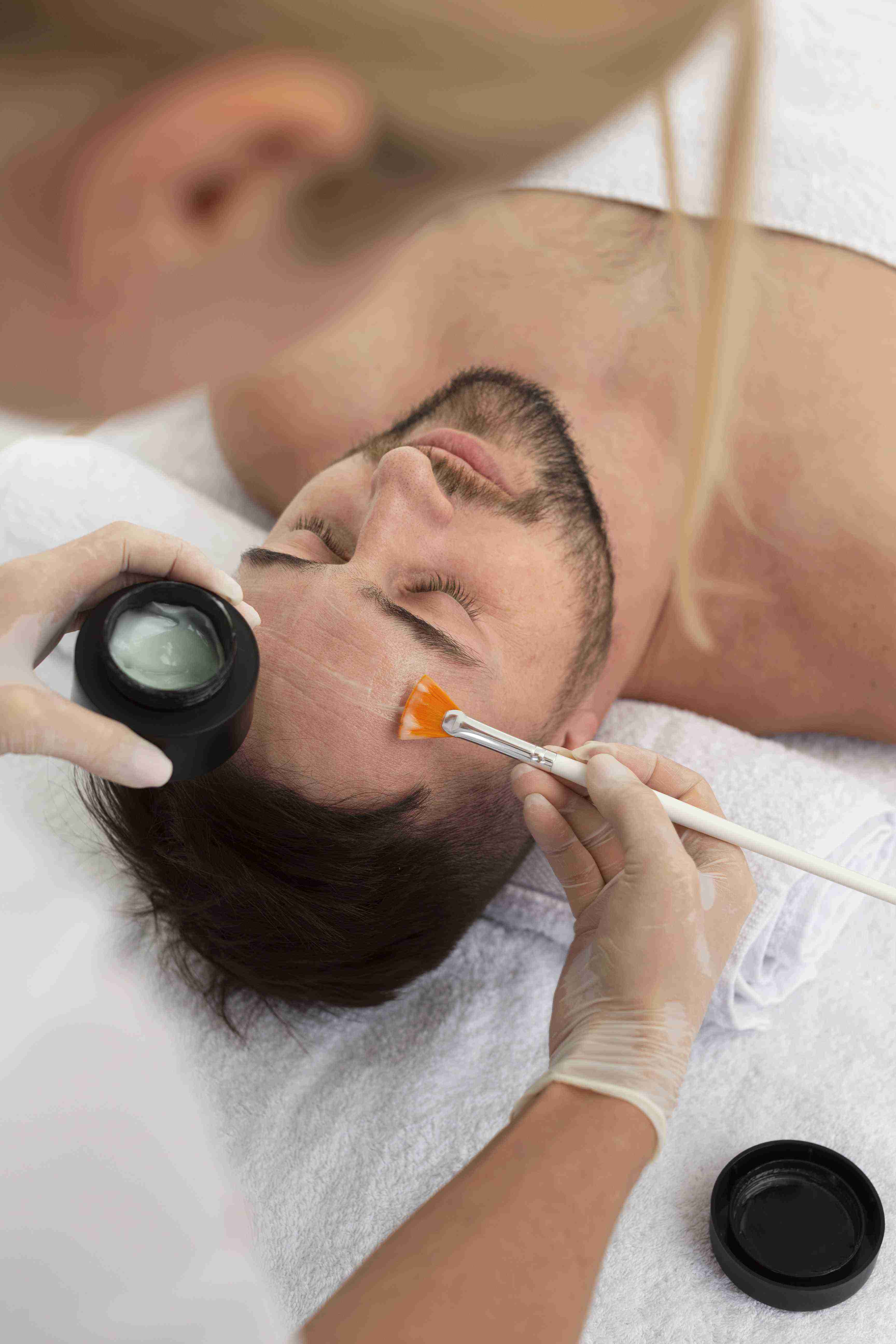
Benefits of Hair Transplant Consultation for Androgenetic Alopecia
The consultation at Claire Derma goes beyond surgical planning to address the medical management of androgenetic alopecia alongside transplantation. Transplanted hairs are permanent because they come from DHT-resistant follicles, but the native hairs surrounding them continue to miniaturise without treatment.
Ideal Candidates for the Treatment
This treatment is ideal for individuals who:
Following the consultation at Claire Derma, you receive a detailed written plan including your Norwood or Ludwig classification, donor density measurements, estimated graft count, recommended technique, expected coverage outcome, and a timeline for the procedure and recovery. We encourage a two-week reflection period before confirming surgery to ensure you have time to consider the information without pressure.
The Treatment Process
01
Consultation & Skin Analysis
The dermatologist assesses acne severity and selects the best peel formulation. Our trichologist conducts a full scalp evaluation with dermoscopy, macrophotography, and donor density measurement. We classify your hair loss stage, calculate available graft supply, and discuss your goals. Blood tests are ordered to rule out conditions affecting surgical candidacy.
02
Preparation
The skin is cleansed, and protective measures are taken for sensitive areas. If medical stabilisation is needed, we prescribe appropriate therapy and monitor for six to twelve months before clearing you for surgery. Pre-operative instructions are provided including medication adjustments, supplement cessation, and logistical planning for the procedure day and recovery period.
03
Peel Application
A customized medium or deep peel solution is applied for controlled penetration. On the procedure day, the surgical team follows the plan designed during your consultation — donor harvesting via FUE or FUT, graft preparation under magnification, and precise recipient site creation at the planned density and angle.
04
Neutralization & Post-Treatment Care
The peel is neutralized, and a soothing recovery serum is applied. Post-operative care instructions cover wound management, sleeping position, activity restrictions, and medication schedules. We schedule follow-ups at one week, one month, and quarterly thereafter.
Expected Results & Recovery
Comprehensive understanding of hair loss condition.
Personalized hair transplant plan tailored to individual needs.
Improved confidence in treatment decisions.
No downtime required for the consultation.
Patients receive detailed post-consultation care guidelines.
Next steps for hair transplant or alternative treatments are clearly defined.
Got Questions?We've Got Answers
Find answers to the most common questions about our treatments, procedures, and recovery process. If you can't find what you're looking for, our support team is always here to help.
Typically, 3–6 sessions, spaced 4–6 weeks apart, yield the best results.
Patients may feel a warm or stinging sensation, but discomfort is manageable.
Peeling and flaking can last between 5–10 days, depending on peel strength.
It significantly reduces acne and breakouts, but maintenance treatments and a proper skincare routine are essential.
Sun exposure must be strictly avoided for at least a week, and broad-spectrum sunscreen is mandatory.
Age itself is not a disqualifier, but hair loss stability is critical. At Claire Derma, we generally advise patients under 25 to delay transplantation because their final pattern of loss is not yet predictable. Transplanting hair into a young scalp where significant further recession is likely means the transplanted hairline may eventually sit as an isolated strip in front of continued thinning.
Graft count depends on the size of the recipient area and the density you want to achieve. At Claire Derma, early frontal recession typically requires 1,500 to 2,500 grafts, moderate loss covering the front and crown needs 2,500 to 3,500, and extensive Norwood V-VI patterns may require 4,000 to 5,000 or more across staged procedures.
The best technique depends on your donor characteristics, graft requirement, and lifestyle preferences. FUE leaves scattered dot scars and suits patients who wear short hairstyles, while FUT yields more grafts per session and is preferred when maximum harvest is needed.
Yes. Transplanted hairs are permanent because they come from DHT-resistant donor follicles, but your native hairs surrounding the transplanted area remain susceptible to androgenetic alopecia. Without ongoing medical therapy, these native hairs will continue miniaturising, potentially creating an unnatural contrast between dense transplanted zones and thinning native areas.