
Introduction to Hair Transplant Consultation for Scarring Alopecia
Scarring Alopecia (Cicatricial Alopecia) is a rare condition where inflammation destroys hair follicles, replacing them with scar tissue. A hair transplant consultation assesses the extent of scarring and evaluates whether transplantation is feasible.
Scarring alopecia — also called cicatricial alopecia — involves permanent destruction of hair follicles replaced by fibrotic scar tissue, which is fundamentally different from non-scarring conditions like androgenetic alopecia. At Claire Derma, the transplant consultation for scarring alopecia carries additional complexity because the scarred recipient tissue has compromised blood supply and may not support graft survival at the same rate as healthy scalp.
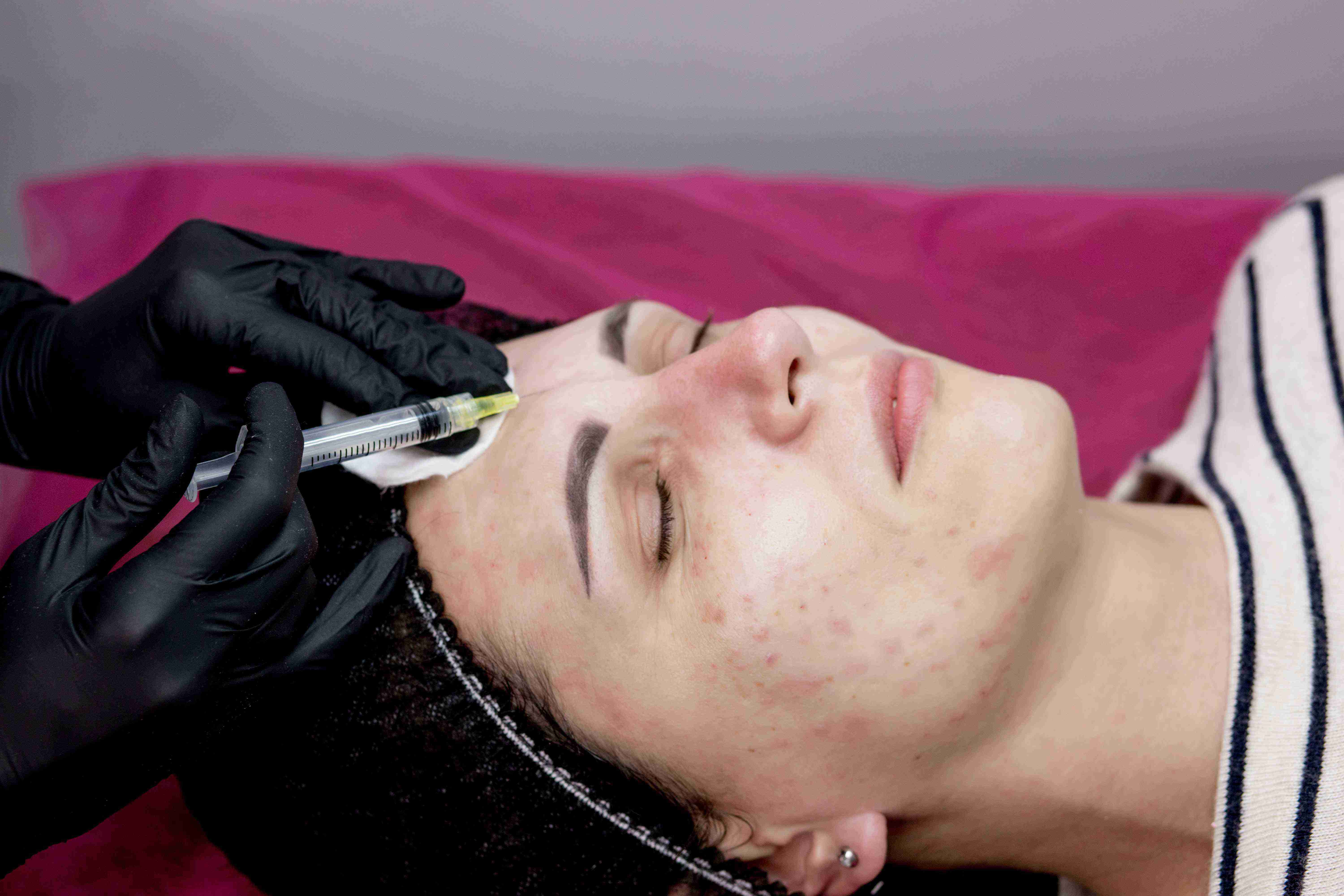
How Hair Transplant Consultation Works
This treatment targets acne and skin congestion by:
The type of scarring alopecia significantly influences transplant planning at Claire Derma. Each condition creates a different pattern of follicle destruction and leaves behind scar tissue with varying characteristics that affect graft survival rates. Burn scars and traumatic scars typically have a well-defined stable border and respond reasonably well to transplantation.

Treating Scarring Alopecia with Hair Transplant
Recipient site preparation in scarring alopecia is more demanding than in standard androgenetic transplant cases. Scar tissue is denser, less vascular, and more resistant to graft insertion than normal scalp skin.
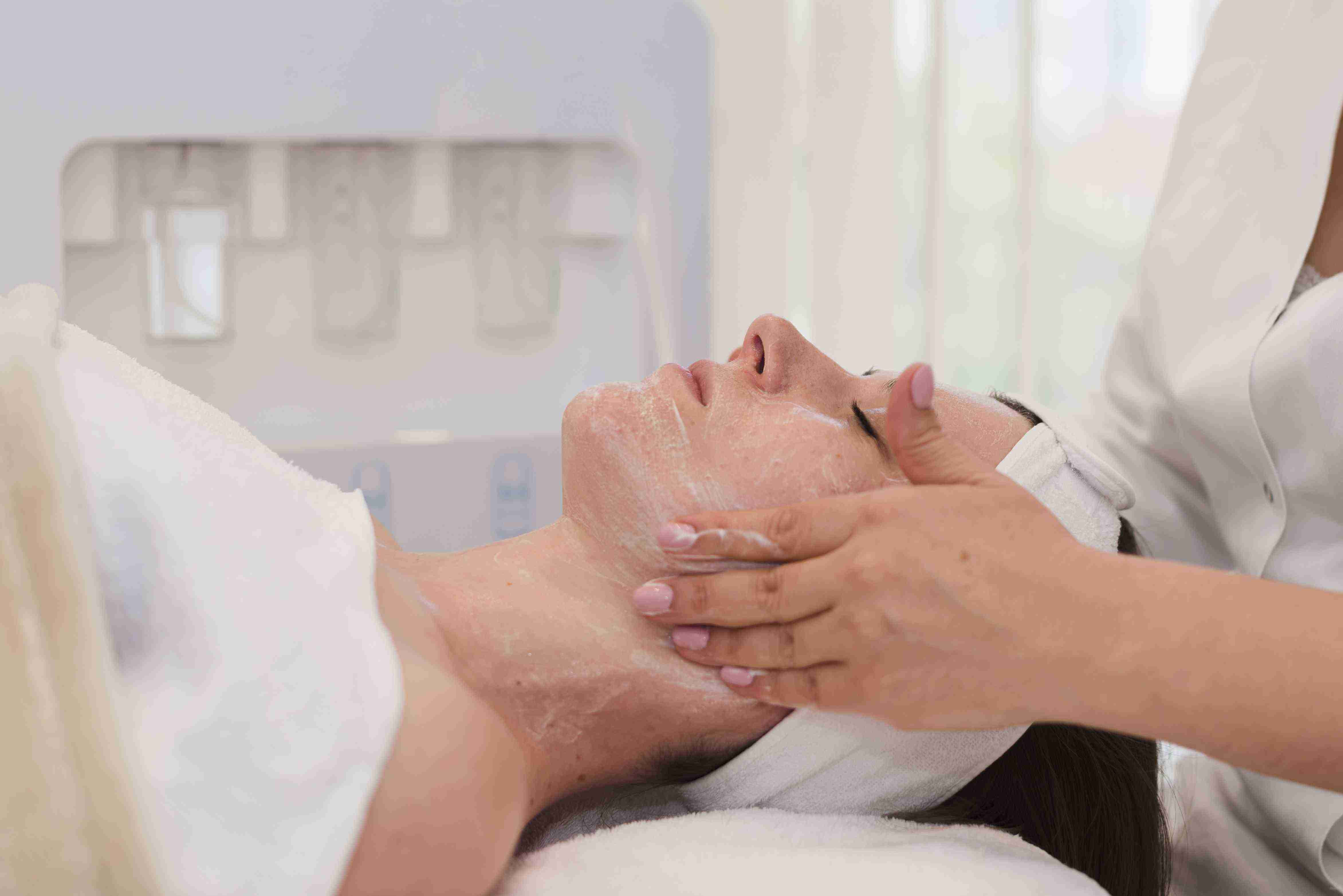
Benefits of Hair Transplant Consultation for Scarring Alopecia
The consultation for scarring alopecia transplantation at Claire Derma provides honest, detailed guidance that prevents patients from pursuing surgery with unrealistic expectations. Scarring alopecia transplants achieve lower density than standard androgenetic procedures, and patients need to understand that the goal is cosmetically meaningful improvement rather than full restoration.

Ideal Candidates for the Treatment
This treatment is ideal for individuals who:
After the consultation at Claire Derma, patients with scarring alopecia receive a detailed written assessment that includes the diagnosis, disease activity status, recipient bed vascularity evaluation, estimated graft count, recommended staging plan, and a realistic projection of achievable density. If the disease is not yet confirmed quiescent, we outline the monitoring schedule and the criteria that must be met before transplant clearance is granted.
The Treatment Process
01
Consultation & Skin Analysis
The dermatologist assesses acne severity and determines the best peel type. Our trichologist evaluates the scarring alopecia type, confirms disease quiescence through dermoscopy and clinical history, and assesses recipient bed vascularity. Donor area density is measured and total available grafts are calculated.
02
Preparation
The skin is cleansed to remove oil and impurities before the treatment. If recipient bed vascularity needs improvement, pre-operative PRP sessions or microneedling are scheduled in the months before surgery. For cases requiring disease quiescence confirmation, serial dermoscopy monitoring continues until the eighteen-month stability threshold is met.
03
Peel Application
A customized chemical peel is applied and left on for controlled exfoliation. The surgical team harvests grafts via FUE — preferred for scarring cases as it allows flexible recipient site placement — and inserts them at conservative density into the scarred recipient bed.
Expected Results & Recovery
Clear understanding of whether transplantation is viable.
Personalized plan with realistic expectations.
Reduced risk of transplant failure or complications.
No downtime required for the consultation..
Detailed post-consultation guidance provided.
Follow-up plan established based on consultation findings.

Got Questions?We've Got Answers
Find answers to the most common questions about our treatments, procedures, and recovery process. If you can't find what you're looking for, our support team is always here to help.
Typically, 3–6 sessions spaced 2–4 weeks apart are recommended.
Chemical peels fade acne scars and dark spots, but deep scars may require microneedling or laser treatments for optimal results.
Most people experience a mild tingling or stinging sensation, but it is tolerable and subsides quickly.
It is recommended to wait at least 24–48 hours before applying makeup to avoid irritation.
Some individuals experience temporary purging before clearing up.
Not all scarring alopecia cases are suitable for transplantation. At Claire Derma, we require confirmed disease quiescence for a minimum of eighteen months before considering surgery. Active lichen planopilaris, frontal fibrosing alopecia, or discoid lupus will destroy transplanted grafts. Heavily fibrosed or avascular scars may also not support graft survival regardless of disease status.
Scar tissue has reduced blood supply compared to healthy scalp because the normal vascular network within the dermis has been replaced by dense collagen fibres during the scarring process. Transplanted follicles depend on revascularisation from the surrounding tissue to survive, and this process is slower and less complete in scar tissue.
Disease quiescence is confirmed through clinical and dermoscopic monitoring over time. At Claire Derma, our trichologists look for the absence of perifollicular erythema, scaling, and progressive hair loss at the scar margins. Dermoscopy should show no active inflammation or loss of follicular openings at the borders. We require documented stability across at least three to four serial assessments over eighteen months.
The risk of disease reactivation exists with autoimmune scarring alopecias like lichen planopilaris and frontal fibrosing alopecia, even after prolonged quiescence. If the disease reactivates, transplanted follicles in the affected zone can be destroyed. At Claire Derma, we monitor patients indefinitely after transplant with periodic dermoscopy and advise continuing any prescribed maintenance therapy.