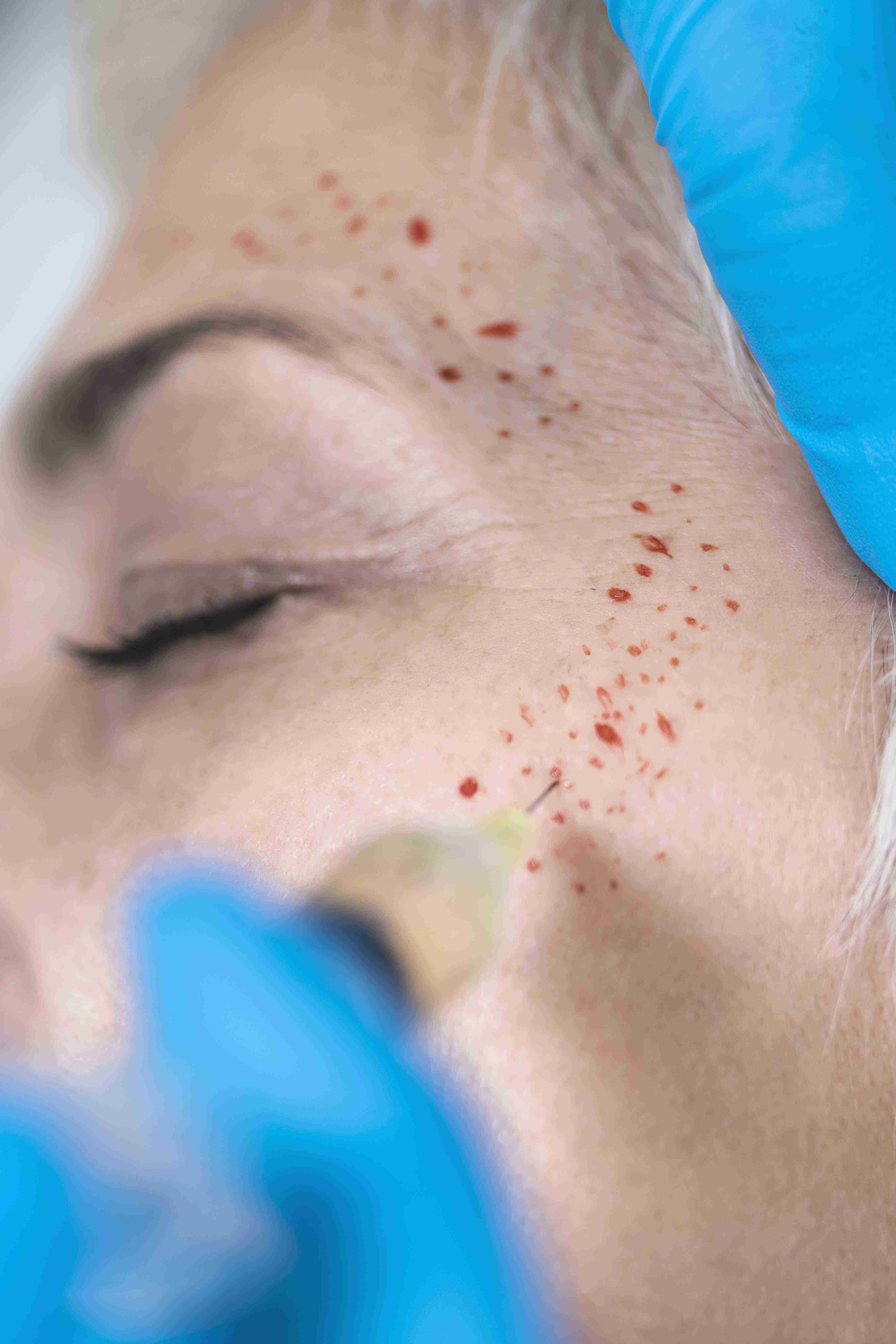
Introduction to Vampire Facelift (PRP Facelift)
The Vampire Facelift, also known as the PRP (Platelet-Rich Plasma) Facelift, is an advanced skin rejuvenation therapy that uses growth factors from the patient’s own blood to stimulate collagen production, cellular regeneration, and skin repair. It is particularly effective for treating pigmentation issues such as melasma, sunspots, post-inflammatory hyperpigmentation, and uneven skin tone by enhancing skin healing, reducing excess melanin production, and promoting an even complexion. Pigmentation disorders occur due to sun exposure, hormonal changes, aging, and skin inflammation. PRP helps restore natural skin tone, smooth texture, and overall radiance without the use of harsh chemicals.
Pigmentation disorders — melasma, post-inflammatory hyperpigmentation, sun spots — result from melanocyte overactivity triggered by UV exposure, hormonal changes, or skin inflammation. Treating pigmentation is notoriously difficult because melanocytes sit at the dermal-epidermal junction and respond unpredictably to aggressive interventions. Vampire facelift therapy offers a different approach: PRP growth factors regulate cellular turnover and promote healthier skin renewal without provoking the inflammatory rebound that worsens many pigmentation conditions.
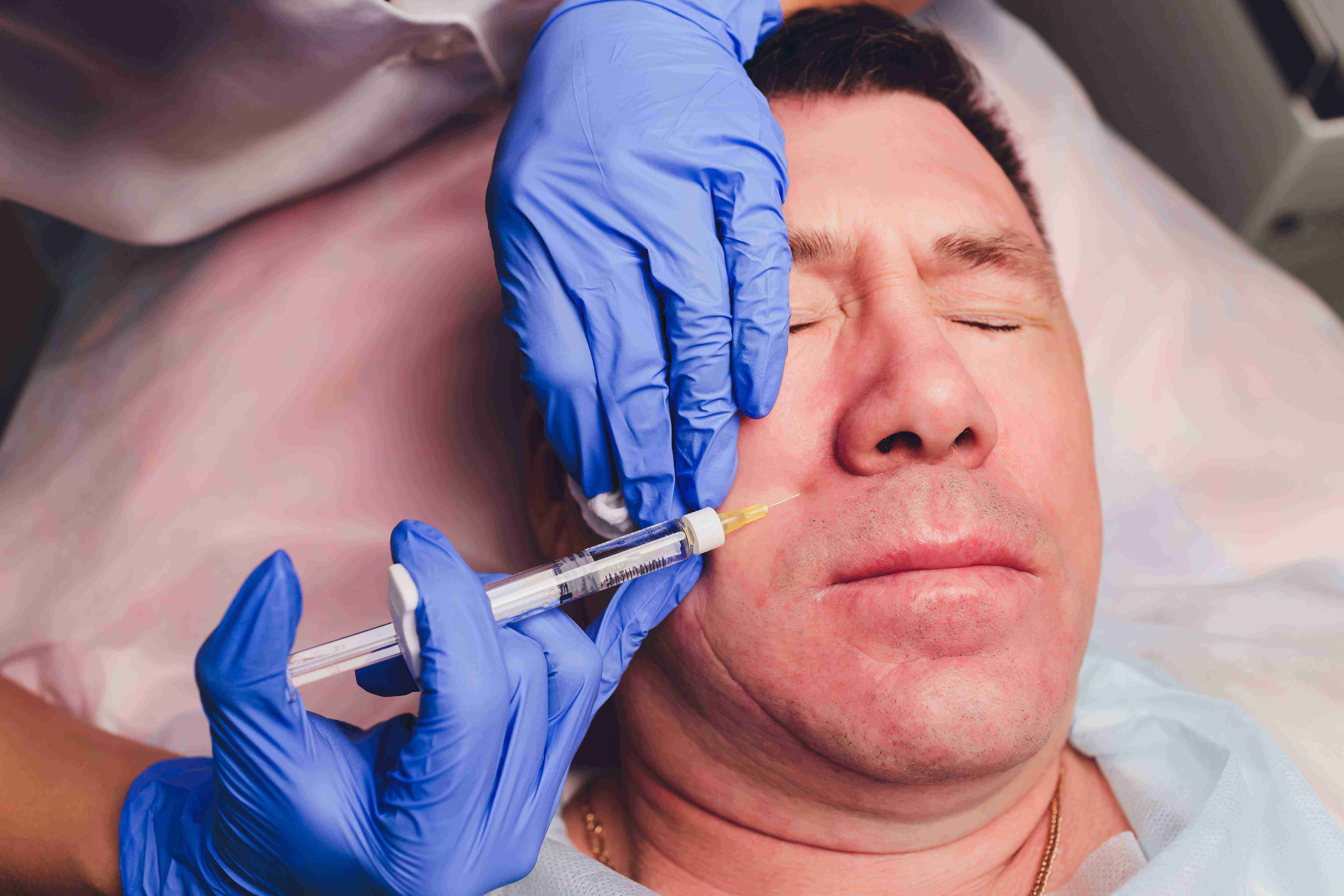
How the Vampire Facelift (PRP Facelift) Works
The treatment involves using platelet-rich plasma (PRP) extracted from the patient’s blood, which is applied to the skin through microneedling or direct injections to boost collagen synthesis, tissue repair, and cellular renewal. The process includes:
Different pigmentation conditions require different PRP approaches. Melasma, driven by hormonal and UV factors, involves excess melanin deposits in both the epidermis and dermis. Post-inflammatory hyperpigmentation from healed acne or eczema tends to be more superficial and predictable in location.
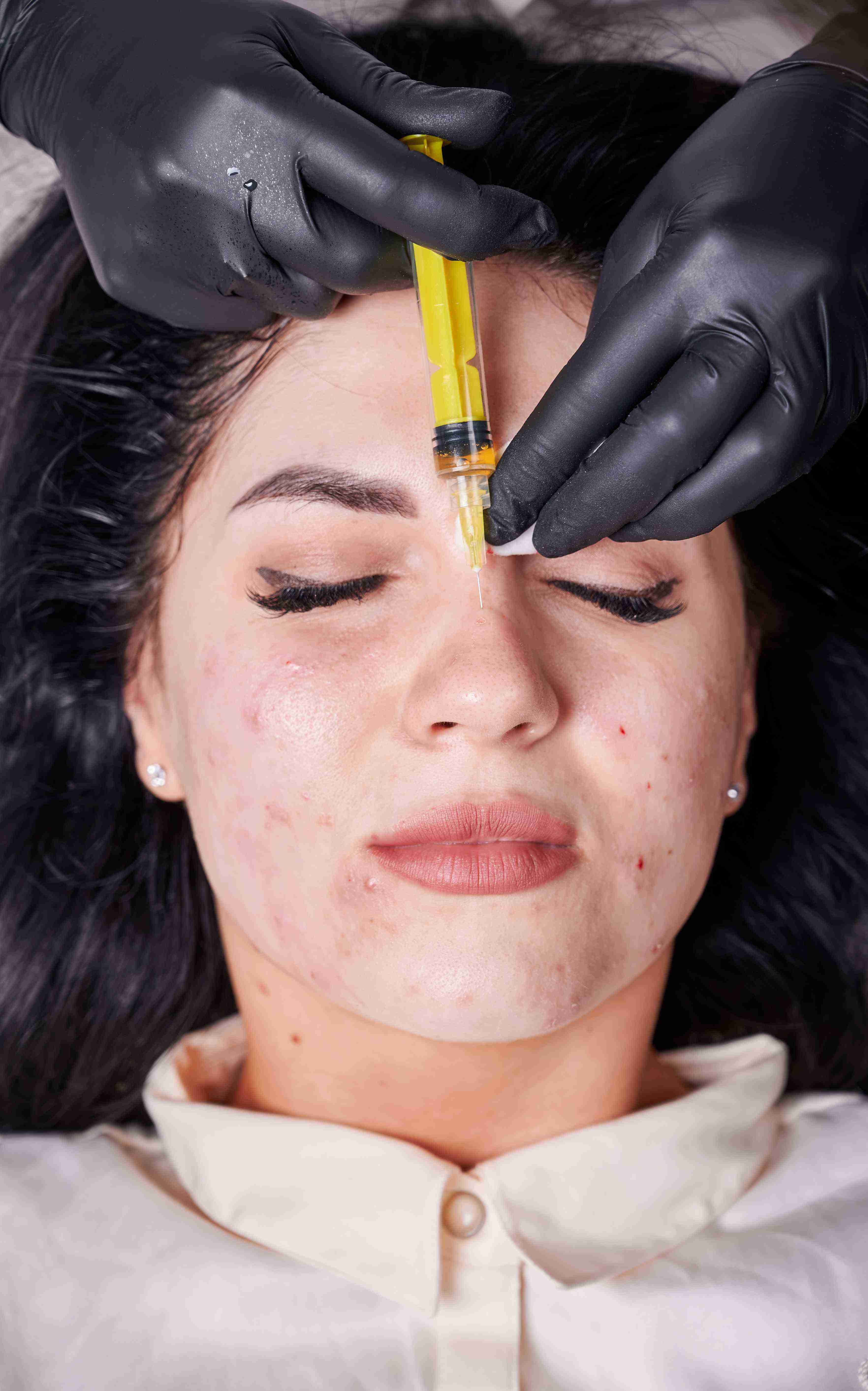
Treating Pigmentation with the PRP Facelift
PRP for pigmentation at Claire Derma uses a preparation and injection approach tailored to avoid triggering further melanocyte activation. We draw 15 to 20 millilitres of blood and process it through dual-spin centrifugation to achieve a concentrated platelet preparation.
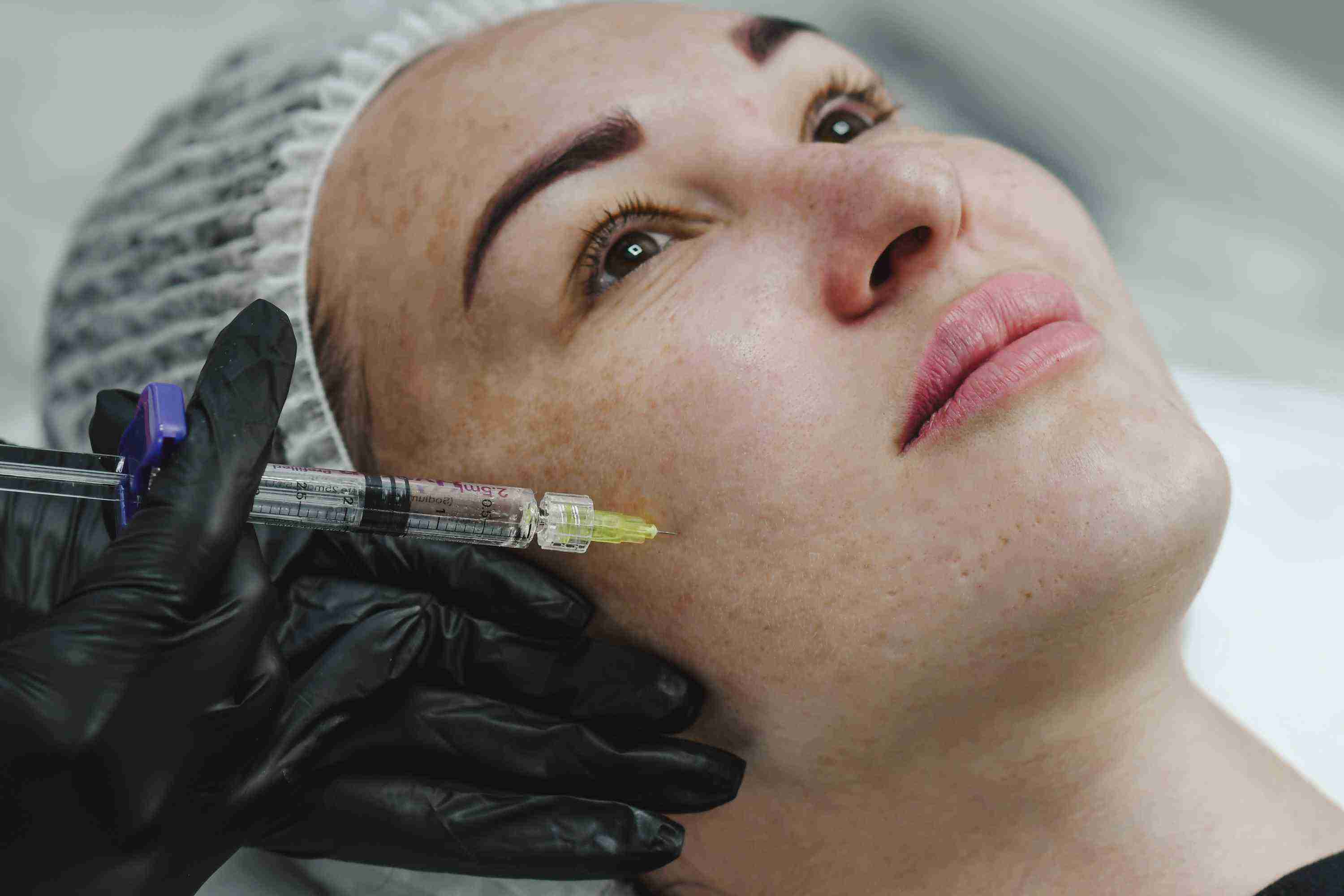
Benefits of the PRP Facelift for Pigmentation
The primary advantage of PRP for pigmentation is its safety profile across all skin tones. Laser treatments for pigmentation carry meaningful risk in Fitzpatrick skin types III through VI — the very patients who experience pigmentation most frequently. Chemical peels must be carefully dosed to avoid rebound hyperpigmentation.
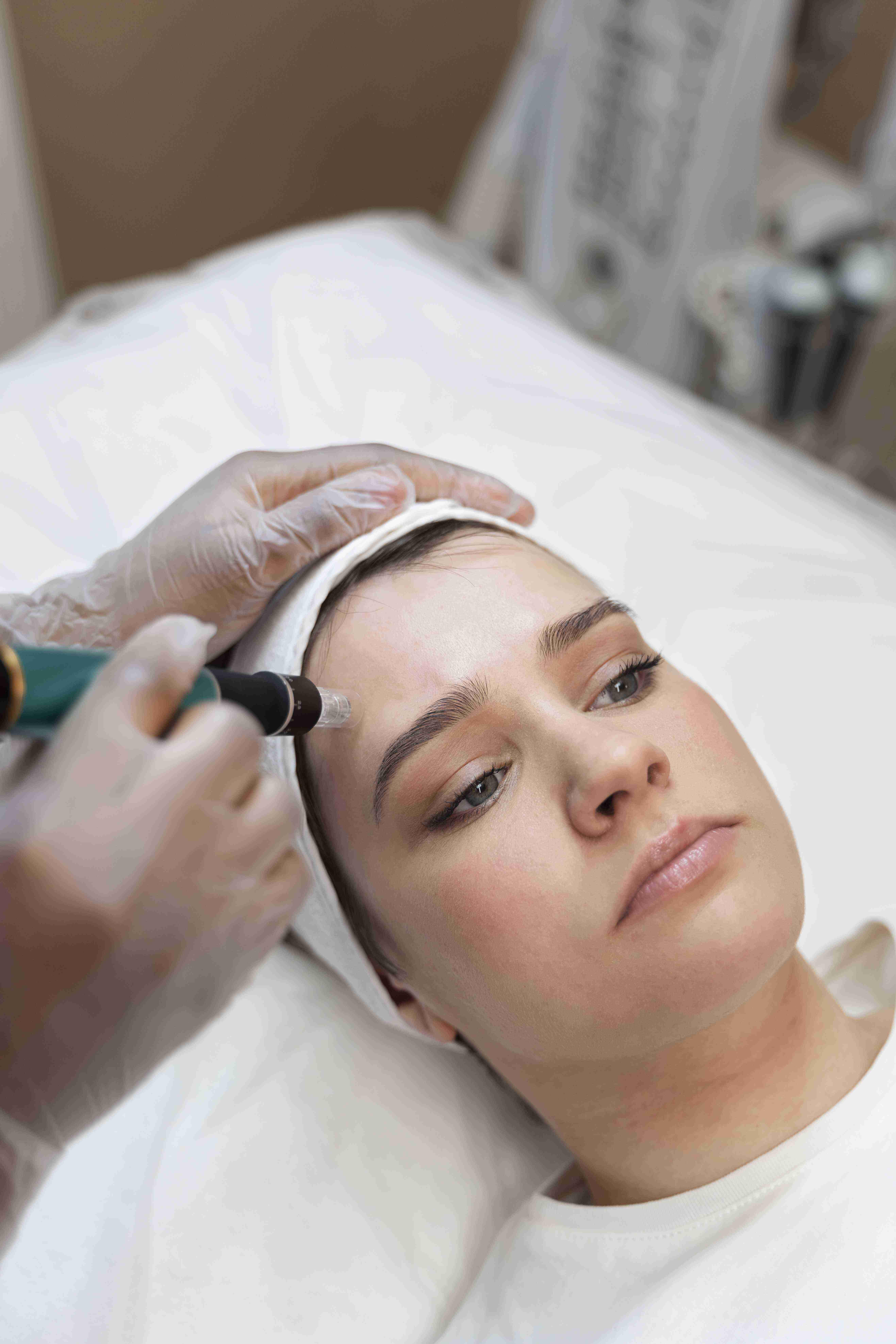
Ideal Candidates for the Treatment
This treatment is ideal for individuals who:
Sun protection is non-negotiable during PRP pigmentation treatment. UV exposure is the primary driver of melanocyte activity, and even excellent PRP results will be undermined without rigorous daily sunscreen use — SPF 50, broad-spectrum, reapplied every two hours during outdoor exposure. At Claire Derma, we emphasise this at every appointment because treatment compliance with sun protection is the single biggest factor determining long-term pigmentation outcomes.
The Treatment Process
01
Consultation & Skin Analysis
A specialist evaluates pigmentation concerns and determines the best treatment plan. Your dermatologist examines pigmentation using Wood's lamp and dermoscopy to determine melanin depth — epidermal, dermal, or mixed. We photograph the affected areas under standardised lighting, review your hormonal health, sun exposure habits, and previous treatments, then design a PRP protocol calibrated to your specific.
02
Blood Extraction & PRP Preparation
A small blood sample is drawn and processed to extract PRP. We draw 15 to 20 millilitres of blood and process it through dual-spin centrifugation. A topical numbing cream is applied to the treatment area during the 15-minute processing time. The PRP is gently activated just before injection.
03
PRP Application
Microneedling technique to penetrate deep layers and boost skin renewal. Direct injection into pigmented areas for targeted correction. Activated PRP is delivered through superficial microinjections at 0.5 to 1.5 millimetre depth using 30- or 32-gauge needles. Injection points are spaced approximately 1 centimetre apart across pigmented zones. The technique prioritises minimal tissue trauma to avoid triggering inflammatory pigmentation.
04
Post-Treatment Care
Mild redness and sensitivity may occur but fade within 24–48 hours. Patients should avoid sun exposure and use SPF to prevent further pigmentation. Mild pinkness at injection sites fades within 12 to 24 hours. Apply prescribed barrier cream and broad-spectrum SPF 50 from the following morning. Avoid retinoids and exfoliating acids for 48 hours. Resume your depigmenting home regimen on day three.
Expected Results & Recovery
Visible pigmentation reduction over 3–6 months as skin regenerates.
Most patients resume normal activities within 1–2 days.
With proper skincare, results last for years.
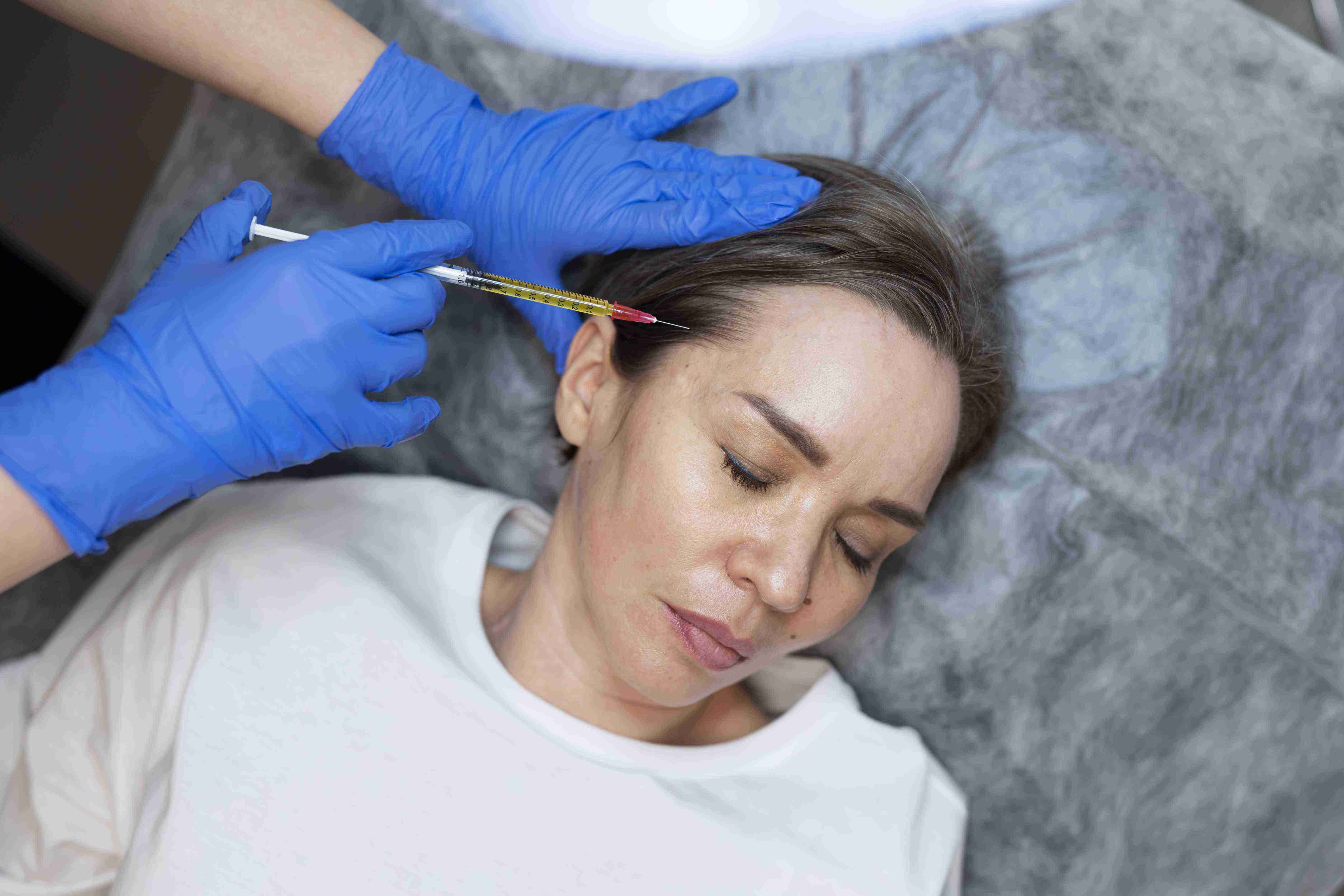
Got Questions?We've Got Answers
Find answers to the most common questions about our treatments, procedures, and recovery process. If you can't find what you're looking for, our support team is always here to help.
Initial improvements in skin tone appear within a few weeks, while full results develop over 3–6 months as collagen rebuilds.
3–5 sessions spaced 4–6 weeks apart provide optimal results, depending on pigmentation severity.
PRP significantly reduces pigmentation, but maintenance treatments and sun protection are essential to prevent recurrence.
PRP stimulates natural skin healing, while peels exfoliate the surface. Combining both treatments can enhance results for stubborn pigmentation.
Yes, PRP can help reduce melasma by controlling inflammation and promoting healthy skin turnover, though results vary based on severity.
Side effects are minimal and may include mild redness, slight swelling, or temporary darkening of pigmented areas, which fade within days.
Yes, PRP can be combined with lasers or microneedling for enhanced pigmentation correction.
When performed correctly with a low-inflammation technique, PRP is one of the safest pigmentation treatments available because it does not generate heat or cause tissue destruction. The risk of worsening pigmentation is very low compared to lasers or medium-depth peels. At Claire Derma, our dermatologists use fine-gauge needles, shallow injection depths, and gentle activation protocols specifically designed for pigmentation-prone skin.
Melasma typically requires four to six PRP sessions spaced three to four weeks apart. Because melasma is a chronic condition driven by hormonal and UV factors, the goal of PRP is to improve the dermal environment and normalise skin turnover rather than permanently eliminate melanin deposits. Most patients see noticeable improvement after three sessions, with continued lightening through the remaining treatments.
It depends on your skin tone, the type of pigmentation, and your risk tolerance. Lasers like Q-switched Nd:YAG can effectively target focal dark spots in lighter skin tones but carry meaningful pigmentation risk for Fitzpatrick types III through VI. PRP is slower-acting but safer across all skin tones because it avoids thermal damage entirely.
Pigmentation conditions like melasma are chronic — the underlying tendency for melanocyte overactivity remains. Without maintenance, pigmentation can gradually return, particularly with sun exposure or hormonal changes. PRP results are maintained most effectively with periodic top-up sessions every three to four months combined with daily sun protection and topical depigmenting agents.